Special Article - Surgical Case Reports
Austin J Surg. 2015;2(1): 1049.
Esophageal Perforation Associated with Massive Pneumoperitoneum after Cardiopulmonary Resuscitation: Case Report
Okumura K1,2* and Suganuma T2
1Department of Surgery, Tokyo-bay Urayasu Ichikawa Medical Center, Japan
2Department of Surgery, Uwamachi General Hospital, Japan
*Corresponding author: Okumura K, Department of Surgery, Tokyo-bay Urayasu Ichikawa Medical Center, 3-4-32, Todaijima, Urayasu, Chiba 279-0001, Uwamachi General Hospital, 2-36, Uwamachi, Yokosuka, Kanagawa 238-0017, Japan
Received: November 24, 2014; Accepted: January 05, 2015; Published: January 07, 2015
Abstract
Cardiopulmonary Resuscitation (CPR) has been performed for the benefit of a successful restoration of a spontaneous circulation although the risk of complications. Despite there are few reports of massive gastric distension causing gastric rupture and pneumoperitoneum after CPR, pneumoperitoneum and esophageal rupture has been rarely reported. We report a case of lower esophageal perforation associated with massive pneumoperitoneum after CPR. Prompt intervention should be performed to repair perforation to decrease the morbidity and mortality.
Keywords: Esophageal perforation; Massive pneumoperitoneum; Cardiopulmonary resuscitation
Introduction
Esophageal perforation can occur spontaneously (Boerhaave syndrome) or as a result of procedures that cause direct esophageal trauma [1]. Despite gastric perforations and pneumoperitoneum after Cardiopulmonary Resuscitation (CPR) have been reported [2], massive pneumoperitoneum and esophageal perforation secondary to CPR has been rarely reported. We report a case of lower esophageal perforation associated with massive pneumoperitoneum after CPR
Case Presentation
A 74-year-old woman with a history of hypertension transferred to our hospital after the cardiopulmonary resuscitation with bag-valve mask for 20 minutes. The patient lost the consciousness without any premonitory symptoms. The patient went back to conscious after the CPR and started to complain an abdominal bloating and an epigastric pain. On examination, the patient had a temperature of 36.2°C, blood pressure of 175/110 mmHg, and a heart rate of 81 bpm. Abdominal examination showed extremely bloating and mild tenderness in the epigastric area with rebound tenderness. Laboratory results showed white cell count of 10100/ul was elevated (normal: 3800–8500/ul) and other serum tests are within normal limits. Abdominal X-ray revealed a massive free air in the peritoneum and mediastinum associated with an enlarged stomach. (Figure 1) Computed tomography scan of the abdomen showed a massive free air in the peritoneum and mediastinum. The diagnosis of gastrointestinal perforation was made, and emergent laparotomy performed. A 4-cm linear tear was seen at right side from lower esophagus to gastroesophageal junction. The tear was sutured by 4-0 PDS-II (Ethicon Inc., NJ and USA), drains were placed in mediastinum and abdominal cavity and a jejunostomy was performed for enteral nutrition. After the operation, the patient had a brain infarction from air embolism, but the patient recovered without other significant complications.
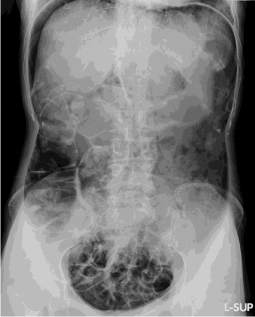
Figure 1: Abdominal X-ray showed massive free air in the peritoneum and
visceral organs such as liver, stomach and colon were seen on this film
(Rigler‘s sign).
Discussion
Spontaneous esophageal perforation related to an elevated intraluminal pressure during vomiting is called the Boerhaave syndrome. The other main cause of esophageal perforation is a direct injury to the esophagus during a medical procedure such as intubation with inadvertent placement of the tracheal tube in the esophagus, nasogastric tube placement, upper GI endoscopy, and transesophageal echocardiography. To our knowledge, our case is the first reported case of esophageal perforation associated with massive pneumoperitoneum after CPR. We cannot prove that CPR directly caused the esophageal tear in the patient since the respiratory parameters of our patient during ventilation were not recorded. Conceivably, the respiratory distress requiring ventilation support may have been caused by a spontaneous esophageal perforation. Nevertheless, the close chronological relationship between CPR and the distention of abdomen in the patient’s status makes this hypothesis unlikely.
Complications involving the abdominal viscera due to CPR occur in about 30% of patients [2]. Common intra-abdominal sequelae of CPR include gastric dilation and liver and spleen injuries, and patients sustain gastric rupture at a rate of 1 in 1000 [2]. Gastric rupture is also a well-documented complication of nasopharyngeal oxygen administration [2]. The predominant site of gastric perforation from CPR is along the lesser curvature of the stomach, possibly because of the decreased number of mucosal folds in this region of the stomach [3]. Esophageal perforation secondary to positive-pressure ventilation applied via a facemask might be plausible due to increased intraluminal pressures sustained during chest compressions [2]. A case of esophageal perforation associated with noninvasive positivepressure ventilation has also been previously reported [1]. In our case, the patient had a gastric distention and massive pneumoperitoneum; these findings supported that lots of oxygen was supplied to her during the CPR, and an excessive positive pressure and increased intraluminal pressures sustained during chest compressions might unfortunately cause the esophageal perforation. A perforated viscus after chest compressions, in patients with multisystem organ failure, most likely would result in death. To prevent these unfortunate events, we should perform CPR by the correct technique to prevent excessive gastric distention. We could save the patient by early recognition and prompt laparotomy to repair perforation. Early intervention is a key of esophageal perforation to decrease the morbidity associated with rupture of a hollow organ if we suspected the perforation.
Conclusion
We present a case describing an esophageal perforation with massive pneumoperitoneum after cardiopulmonary resuscitation. Clinicians should be aware that CPR could cause various complications, which may include an esophageal perforation.
Consent: The patient gave written consent that the patient´s case could be used as the basis for this manuscript.
References
- Van de Louw A, Brocas E, Boiteau R, Perrin-Gachadoat D, Tenaillon A. Esophageal perforation associated with noninvasive ventilation: a case report. Chest. 2002; 122: 1857-1858.
- Hahn CD, Choi YU, Lee D, Frizzi JD. Pneumoperitoneum due to gastric perforation after cardiopulmonary resuscitation: case report. Am J Crit Care. 2008; 17: 388, 386-387.
- Demos Nj, Poticha Sm. Gastric rupture occurring during external cardiac resuscitation. Surgery. 1964; 55: 364-366.