
Case Report
Austin J Pulm Respir Med 2016; 3(1): 1041.
Non Resolving Lung Abscess - The Hidden Truth
Sandhya AS¹, Prajapat B²* and Bherwani S³
¹Department of Chest and Tuberculosis, Pt. B D Sharma Postgraduate Institute of Medical Sciences, India
²Department of Pulmonary and Critical Care Medicine, Pt. B D Sharma Postgraduate Institute of Medical Sciences, India
³Department of Medicine, Lady Hardinge Medical College, India
*Corresponding author: Brijesh Prajapat, Department of Pulmonary and Critical Care Medicine, Pt. B D Sharma Postgraduate Institute of Medical Sciences, India
Received: April 20, 2016; Accepted: May 31, 2016; Published: June 01, 2016
Abstract
Pulmonary embolism rarely present with infarction and cavitation and when it does the condition mimics other common conditions like tuberculosis, malignancy, necrotizing pneumonia etc. that creates a diagnostic dilemma even for an astute clinician. A high degree of suspicion must be kept in mind while dealing with non responding lung abscess.
Keywords: Lung abscess; Pulmonary embolism; Cavity; Lung cancer; Tuberculosis
Introduction
Pulmonary embolism is the most serious clinical presentation of venous thromboembolism and is a major cause of morbidity, mortality and hospitalizations. The epidemiology is difficult to determine as most of the cases remain undiagnosed. It does not commonly present with cavitation because of the dual blood supply of the lung; however, cavitation may complicate 4–7% of all pulmonary infarctions. Pulmonary cavitations are usually due to infections, malignancies or immunological diseases and a high index of suspicion is needed to diagnose pulmonary embolism in these cases. We present a case of an 80 yr old male patient who presented with chest pain, fever and hemoptysis with chest x-ray showing cavitation. Patient was treated on the lines of lung abscess but CT scan done showed pulmonary embolism in the right main pulmonary artery.
Case Report
An 80-year-old male presented to the emergency department with chief complaints of right sided chest pain for 25 days, cough with expectoration and fever of 15 days duration and hemoptysis for 5 days. Patient had developed acute onset of right sided pleuritic chest pain followed by cough with whitish expectoration which later turned purulent. Patient also had intermittent fever associated with chills but no rigors. Patient developed hemoptysis 5 days before his presentation to the emergency. For the above complaints he took medications from local medical practitioner but was not relieved. As his breathlessness and general condition worsened he presented to the emergency department of our hospital. His past history was unremarkable with no prior history of tuberculosis, any prolonged medication or hospitalization or surgical intervention. There was no history of orthopnea or Paroxysmal nocturnal dyspnoea. Patient was a chronic smoker having 60 years history of hukka and bidi smoking and took alcohol occasionally.
On examination patient was febrile, alert, of average built with good nutritional status. He was normotensive with HR of 98/min, RR of 28/min and SpO2 of 94% on room air. Auscultation revealed coarse crepts on right side. Laboratory investigations showed hemoglobin of 14 g/dl, total leucocyte count of 14000/cumm, blood urea of 122 mg/dl and serum creatinine of 0.93 mg/dl. Liver function tests were within normal limits (SGPT-22IU, SGOT- 30IU, ALK phosphatase – 45IU). Chest X-ray (Figure 1) showed a thick walled cavity involving the right upper and middle zone with air fluid level and surrounding consolidation. A diagnosis of right lung abscess was made and patient started on intravenous antibiotics along with symptomatic treatment. His HIV, HbsAg and HCV were non reactive. Sputum for AFB was negative and sputum for pyogenic culture showed citrobacter and his antibiotics were changed according to the sensitivity report. Patient had relief in his fever, cough and hemoptysis and his chest X-ray (Figure 2) also started showing resolution. But there was no significant improvement in his breathlessness and generalized weakness. Contrast enhanced CT scan of the chest was done when patient remained symptomatic after two weeks of antibiotic therapy. CT scan (Figure 3) revealed pulmonary embolism involving the right main pulmonary artery incompletely occluding the artery. His troponin T was negative, CPK-MB was 92 u/l and serum pro BNP level was 124.7. Echocardiography showed RA/RV dilated with grade 1 diastolic dysfunction. The diagnosis was revised as sub massive pulmonary embolism with infected cavity and he was started on enoxaparin and antibiotics as per his sensitivity reports.
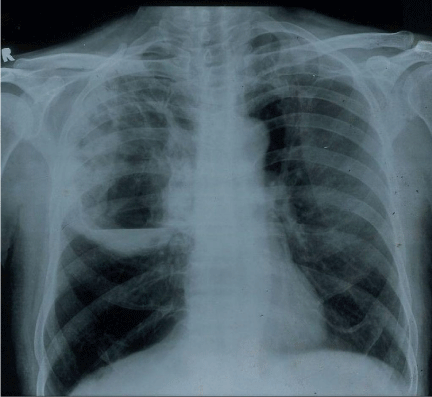
Figure 1: Chest X-ray PA view shows a right sided large abscess with air fluid
level at the time of presentation.
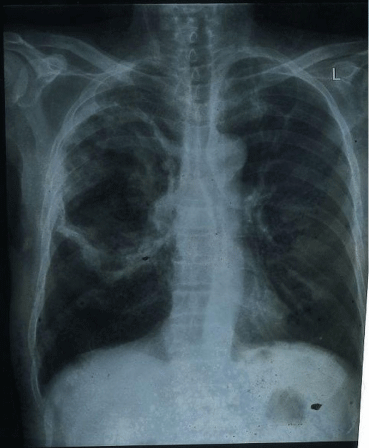
Figure 2: Chest x-ray after 7 days shows resolution with thinning of cavity
wall and no air fluid level.
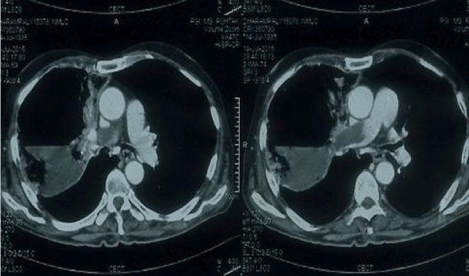
Figure 3: Contrast CT of chest shows filling defect of contrast in right
pulmonary artery suggestive of embolus in the right pulmonary trunk.
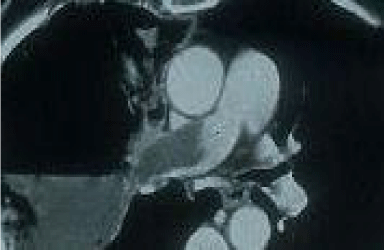
Figure 4: Enlarged view of pulmonary trunk which shows filling defect of
contrast in right pulmonary artery.
Discussion
Pulmonary infarction occurs in ~10% of cases of pulmonary embolism, the low incidence being due to dual pulmonary blood flow, as well as oxygenation by ventilation [1]. Pulmonary infarction may present with complications like cavitation, pneumonia, abscess, pneumothorax, empyema, hemorrhage and bronchopleural fistula. Cavitation may complicate 4-7% of these cases [2]. Cavitation after pulmonary infarcts may result from either aseptic necrosis of the infarcted lung or from secondary bacterial infection with subsequent abscess formation [3]. In our patient the clinical, radiological and laboratory features suggest pulmonary infarction followed by secondary bacterial infection as the cause of cavitation and abscess formation. Patients with underlying chronic heart and lung diseases and immunocompromised states are more prone to have cavitation following pulmonary infarct. Our patient was 80 years old and was a chronic smoker.
Differentiating between infection and embolism as the cause of cavitation clinically remains a diagnostic dilemma. Clinical and radiographic similarities of bacterial pneumonia and pulmonary infarction are the chief source of diagnostic confusion between both entities. Both conditions may present with dyspnea, cough, hemoptysis, chest pain and fever. Physical signs are nonspecific. High grade fever with preceding upper respiratory tract infection may support infective diagnosis while patients with embolism will have more dyspnea, chest pain, hypotension and signs of pulmonary hypertension and right heart failure. Total leukocyte count may be raised in both conditions. Other blood investigations do not have any discriminatory value [4]. Sputum cultures may reveal organism in bacterial abscess but will also be positive in infected cavity following embolism as in our case. Gram negative bacteria are most commonly seen in secondary infection [5].
Chest x-ray may show a cavity in both cases. Cavitation following pulmonary embolism usually occurs in the right side predominantly in the apical or posterior segment of upper lobe or apical segment of lower lobe [6]. They may occur with dilated pulmonary arteries with oligemia in affected side. A regular cavity size, irregular cavity line with no fluid level may suggest bland cavity. Our patient presented with cavity in right upper lobe with irregular cavity line and air fluid level suggesting secondary infection. The greater the size of infarct, more the chances of its centre being hypoxic and necrotic. Pulmonary infarct more than 4×4 cm has a greater tendency to cavitate [6].
Pulmonary angiography or CT pulmonary angiography is the most definitive method of diagnosing. Echocardiography will reveal right ventricular dilatation, septal deviation of right ventricle with tricuspid regurgitation [7].
Delaying the right treatment may lead to high mortality rates. The mortality rate is as high as 41% and 73% for noninfected and infected cavitary pulmonary infarcts, respectively [8]. Anticoagulants and antibiotics are the mainstay of therapy. Our patient was managed with subcutaneous heparin, oral warfarin and parenteral antibiotics. He was discharged on oral warfarin maintaining an International Normalized Ratio 2-3. As the patient was hemodynamically stable with insignificant right ventricular dysfunction thrombolysis was not considered.
Conclusion
Infected cavitary pulmonary infarct is a rare and frequently misdiagnosed disease entity. Due to similar clinical and radiographic picture differentiation between cavitary pulmonary infarct and multiple complications or other diseases like septic emboli, necrotizing pneumonias, cavitary fungal infections, tuberculosis, malignancy (both primary and metastatic to lungs) and vasculitides (granulomatosis with polyangiitis) can pose a real challenge. A high index of clinical suspicion is needed for diagnosis especially antibiotics unresponsive cases. Pulmonary CT angiography is the best method of diagnosis. Anticoagulant and antibiotic treatment in the cases of infected cavitary pulmonary infarct must be started immediately after the diagnosis is established.
References
- Urano, Shibayama Y, Fukunshi K, Nariyama K, Ohsawa N. Interruption of pulmonary arterial flow with inadequate ventilation leads to pulmonary infection. Virchows Arch. 1996; 427: 607-612.
- Huang LH. Pulmonary Infarction. 2008.
- Morgenthaler TI, Ryu JH, Utz JP. Cavitary pulmonary infarct in immunocompromised hosts. Mayo Clin Proc. 1995; 70: 66-68.
- Fred HL. Bacterial pneumonia or pulmonary infarction? Dis Chest. 1969; 55: 422-425.
- Rajagopala S, Devaraj U, D’Souza G. Infected cavitating pulmonary infarction. Respir Care. 2011; 56: 707-709.
- Wilson AG, Joseph AE, Butland RJ. The radiology of aseptic cavitation in pulmonary infarction. Clin Radiol. 1986; 37: 327-333.
- Geibel A, Zehender M, Kasper W, Olschewski M, Klima C, Konstantinides SV. Prognostic value of the ECG on admission in patients with acute major pulmonary embolism. Eur Respir J. 2005; 25: 843-848.
- Djordjevic I, Pejcic T. Cavitary Pulmonary Infarct: The Differential Diagnostic Dilemma – A Case Report.Clinic for lung diseases. Clinical Center – Nis. Serbia.