
Case Series
Austin J HIV/ AIDS Res. 2016; 3(1): 1019.
Pulmonary Kaposi Sarcoma: A Case Report and Review of the Literature
Egwuonwu SO*
Department of Internal Medicine, Southwestern Medical Center, Lawton, Oklahoma
*Corresponding author: Egwuonwu SO, Department of Internal Medicine, Southwestern Medical Center. Lawton. Oklahoma
Received: January 04, 2016; Accepted: January 22, 2016; Published: January 25, 2016
Abstract
Kaposi sarcoma is the most common neoplasm associated with Human Immunodeficiency Virus (HIV) infection. It commonly affects the skin and visceral organs. The commonest organs affected are the lungs and gastrointestinal tract. A 40 year old HIV positive homosexual male presented with fever, intractable cough and dyspnea. He was noted with non blanching purple skin lesions all over his body. CD4 count was 63 cells/mm3and viral load of 50,000. Computed Tomography revealed multiple opacities and pulmonary nodules. Biopsy of the skin lesion confirmed Kaposi sarcoma. Bronchoscopy revealed multiple endobronchial KS lesions. Biopsy of endobronchial lesion confirmed pulmonary KS. He was initiated on highly active antiretroviral therapy (HAART). Chemotherapy was subsequently added. He responded well to treatment.
Pulmonary Kaposi sarcoma can occur with or without cutaneous Kaposi sarcoma lesions. HAART is the mainstay of treatment.
Keywords: Pulmonary Kaposi sarcoma; Human immunodeficiency virus; Highly active antiretroviral therapy; Bronchoscopy
Abbreviations
KS: Kaposi Sarcoma; HIV: Human Immunodeficiency Virus; CT: Computed Tomography; HAART: Highly Active Antiretroviral Therapy; HHV 8: Human Herpes Virus 8; BAL: Bronchoalveolar Lavage; CD4: Cluster of Differentiation 4.
Introduction
Kaposi sarcoma is the commonest neoplasm associated with Human Immunodeficiency Virus (HIV) Infection. In the United States, its prevalence has declined since the advent of Highly Active Antiretroviral Therapy (HAART). The clinical course of HIVRelated Kaposi sarcoma could be indolent with minor cutaneous or lymph node disease or aggressive with extensive skin and visceral involvement. The lungs and gastrointestinal tract are the commonest systems affected. This article describes pulmonary Kaposi sarcoma with a review of clinical features, diagnosis and treatment.
Case Presentation
A 40 year-old HIV positive homosexual male not on HAART Therapy presents with a 1month history of intractable cough, hemoptysis and shortness of breath. He had associated night sweats, 5 month history of generalized skin lesions and 30 pound weight loss over 1 year. Physical examination revealed a non blanching purple skin lesion on the face, arms, legs and soles of both feet. Examination of the oral mucosa revealed thrush in the soft and hard palate and dark purple lesions in the posterior pharynx. Breath sounds were decreased bilaterally. Cardiovascular and abdominal exam were unremarkable. White blood cell and platelet counts were within normal limits. He was anemic with hemoglobin of 10 g/dl (14 – 17g/dl). Viral load was 50,000 and CD4 Count was very low at 63 cells/mm3 (500 – 1500 cells/mm3). Chest x-ray showed multiple nodular opacities in both lung fields. Computed tomography of the chest revealed multiple diffuse opacities and pulmonary nodules (Figure 1). Skin biopsy confirmed the cutaneous lesions to be Kaposi sarcoma. Bronchoscopy revealed purple plaques throughout most of his airways. Endobronchial biopsy confirmed Kaposi sarcoma. Given his clinical history, laboratory studies, radiologic imaging and bronchoscopy findings and biopsy result, he was diagnosed with extensive cutaneous and pulmonary Kaposi sarcoma. He was started on HAART therapy with subsequent addition of 8 cycles of liposomal doxorubicin. He responded well to treatment and still alive and well 2 years after diagnosis.
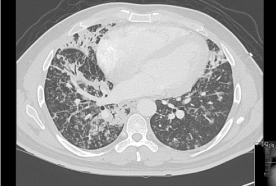
Figure 1: CT showing multiple lung nodules and opacities.
Discussion
Kaposi sarcoma was first described by Moritz Kaposi in 1972. It is a low grade multicentric vascular tumor involving blood vessels and lymph nodes. AIDS- Related Kaposi sarcoma is mostly seen in homosexual or bisexual men. Human Herpes Virus 8 (HHV- 8) has been causally linked to Kaposi sarcoma. Kaposi sarcoma starts off with a polyclonal angioproliferative reaction towards HHV-8. Eventually these polyclonal cells change to oligoclonal cell populations that undergo malignant transformation. The use of Highly Active Antiretroviral Therapy (HAART) has led to a decline in the incidence of KS from 30 per 1000 patient years to 0.03 per 1000 patient years [1]. Kaposi sarcoma commonly affects the skin. The lungs and gastrointestinal tract are the most common visceral organs affected. Although 80- 90 % of pulmonary Kaposi sarcoma occur with extensive cutaneous involvement [2], only 45 % of cutaneous Kaposi sarcoma HIV patient present with pleural or parenchymal disease.
In 15.5 % of patients with pulmonary KS, there is absent cutaneous disease [3]. Kaposi sarcoma of the lungs may be asymptomatic and picked up incidentally by radiologic imaging or bronchoscopy. Common symptoms of pulmonary KS include dry cough, pleural chest pain, hemoptysis, fever, dyspnea, respiratory failure and upper airway obstruction. A thorough examination of the skin and mucus membrane is essential in the evaluation of a patient with suspected pulmonary Kaposi sarcoma. Patients with Kaposi sarcoma typically have a low CD4 cell count (<100 cells/mm3) [4] and a high viral load count >10,000 copies. Chest x-ray findings include reticular opacities or parenchyma nodules in a peribronchovascular pattern of distribution [5]. Unilateral or bilateral pleural effusion may occur. Chest x-ray may be normal in pulmonary KS. The commonest computed tomography findings include interstitial thickening and pulmonary nodules in a peribronchovascular pattern. Other CT findings include airspace consolidation, interlobular septal thickening, ground glass opacities (which may suggest alveolar hemorrhage), mediastinal adenopathies and pleural effusion [2,3,6]. The main essence of bronchoscopy with bronchovascular lavage is to examine the airways for any endobronchial KS lesions and obtain Bronchoalveolar Lavage (BAL) sample for bacterial stain and culture, fungal studies, mycobacterial studies and cytology exam for malignancy. This helps evaluate for opportunistic infections and malignancy. Kaposi sarcoma lesions typically involves the trachea, bronchial system, lung parenchyma and visceral pleura. Biopsy of endobronchial lesions has an increased risk of hemorrhage in about 30% of patients [7,8], so biopsy should be avoided when KS is very likely. The finding of KS lesions below the carina usually indicates parenchymal involvement [9].
The diagnosis of pulmonary KS can be made in the right setting, from a combination of clinical, laboratory, radiologic imaging and bronchoscopic findings.
Endobronchial or transbronchial biopsies are required in most other instances to confirm the characteristic Kaposi sarcoma histologic feature as diagnosis cannot be made from cytology samples
Histologic features of Kaposi sarcoma include angiogenesis, chronic inflammation and spindle cell proliferation. Spindle cells stain positive for CD34 and CD31. Polymerase chain reaction and immunostaining for HHV 8 can be done on biopsy specimens to confirm diagnosis of Kaposi sarcoma.
HAART is the cornerstone of therapy in AIDS -related pulmonary Kaposi sarcoma. Since the advent of HAART, median survival time has increased from 4 months to 1.6 years in pulmonary KS patients [10]. These antiretroviral drugs cause partial or complete regression of KS lesions, decrease cases of KS and protect HIV patients from developing KS [11].
Addition of chemotherapy is warranted when pulmonary Kaposi sarcoma patients present with symptoms or disease progression despite highly active antiretroviral therapy. Chemotherapy agents used for Pulmonary KS include pegylated liposomal doxorubicin, liposomal daunorubicin, vincristine, vinblastine and bleomycin.
Thoracentesis should be performed for large pleural effusion in addition to HAART and chemotherapy. With recurrent pleural effusion, placement of an indwelling pleural catheter or talc pleurodesis can be performed.
Conclusion
Pulmonary Kaposi sarcoma can occur with or without cutaneous Kaposi lesions. The diagnosis of pulmonary Kaposi can be made by a combination of clinical, laboratory, and radiologic findings together with bronchoscopic and transbronchial biopsy results. The main stay of treatment is Highly Active Antiretroviral Therapy (HAART).
References
- Portsmouth S, Stebbing J, Gill J, Mandalia S, Bower M, Nelson M, et al., A comparison of regimens based on non-nucleoside reverse transcriptase inhibitors or protease inhibitors in preventing Kaposi’s sarcoma. AIDS. 2003; 17: F17-22.
- Huang L, Schnapp LM, Gruden JF, Hopewell PC, Stansell JD. Presentation of AIDS -related pulmonary Kaposi’s sarcoma diagnosed by bronchoscopy. Am J Respir Crit Care Med.1996; 153:1385-90
- Restrepo CS, Martinez S, Lemos JA, Carrillo JA, Lemos DF, Ojeda P, et al., Imaging manifestations of Kaposi’s sarcoma. Radiographics 2006; 26: 1169-1185.
- Gill PS, Akil B, Colleti P, Rarick M, Loureiro C, Bernstein-Singer M, et al. Pulmonary Kaposi’s sarcoma: clinical findings and results of therapy. Am J Med 1989; 87: 57-61.
- Lanoy E, Spano JP, Bonnet F, Guiguet M, Boue F, Cadranel J, et al., The spectrum of malignancies in HIV-infected patients in 2006 in France: the ONCOVIH study. Int J Cancer 2011; 129: 467 -475.
- Khalil AM, Carette MF, Cadranel JL, Mayaud CM, Bigot JM. Intrathoracic Kaposi’s sarcoma. CT findings. Chest 1995; 108:1622-1626.
- Meduri GU, Stover DE, Lee M, Myskowski PL, Caravelli JF, Zaman MB. Pulmonary Kaposi’s sarcoma in the acquired immune deficiency syndrome. Clinical, radiographic and pathologic manifestations. Am J Med 1986; 81: 11-8.
- Aboulafia DM. The epidemiologic, pathologic and clinical features of AIDS-associated pulmonary Kaposi’s sarcoma. Chest 2000; 117: 1128.
- Gruden JF, Huang L, Webb WR, Gamsu G, Hopewell PC, Sides DM. AIDS-related Kaposi sarcoma of the lung: radiographic findings and staging system with bronchoscopic correlation. Radiology 1995; 195: 545-552.
- Palmieri C, Dhillon T, Thirlwell C, Newsom-Davis T, Young AM, Nelson M, et al., Pulmonary Kaposi sarcoma in the era of highly active antiretroviral therapy. HIV Med 2006; 7: 291-293.
- Mosam A, Shaik F, Uldrick TS, Esterhuizen T, Friedland GH, Scadden DT, et al., A randomized controlled trial of highly active antiretroviral therapy versus highly active antiretroviral therapy and chemotherapy in therapy naïve patients with HIV associated kaposi sarcoma in South Africa. J Acquir Immune Defic Synd 2012; 60: 150-157.