Abstract
Purpose: This work is aimed at evaluating the effectiveness of medical intervention in encouraging tobacco quitting, controlling for the characteristics of those who try to quit.
Methods: Using data from the Global Adult Tobacco Survey (GATS) in Argentina (2012), Brazil (2008) and Uruguay (2009), logit models are estimated taking into account the characteristics of smokers and medical intervention in consultation as explanatory variables of motivation to quit tobacco.
Results: In Uruguay and Brazil controlling for smoker’s characteristics, like age, gender, education, type of employment, and smoking frequency, those that have consulted a doctor and within this group who have received brief medical advice are more likely to try quitting. In Uruguay and Argentina we find that people under 45 years have a higher rate of intention to quit than average, although they receive a smaller proportion of brief medical advice than other age groups.
Conclusions: Most intention to quit in Uruguay and Argentina in groups of young people cannot relate to medical advice, so it is postulated that other tobacco control policies such as health warnings on cigarettes packs, smoke free areas, to which in the case of Uruguay tobacco tax increases and the ban on advertising, promotion and sponsorship of tobacco products are added. The cost-effectiveness of tobacco cessation programs tobacco could improve if the proportion of people receiving brief medical advice in the younger age tranches is increased and are designed comprehensive programs that include the management of other risks.
Keywords: Tobacco cessation; Brief medical advice; Cost-effectiveness; Tobacco use disparities; Medical intervention effectiveness
Abbreviations
GATS: Global Adults Tobacco Survey; ANOVA: Analysis of Variance; OR: Odds ratio
Introduction
The consumption of tobacco is the most important cause of preventable deaths worldwide [1], and the prospects are that the epidemic is concentrated in developing countries, because the tobacco industry has focused its efforts to increase sales in them because they have a huge population with rising incomes, a high percentage of young people, and fewer regulations than developed countries. The World Health Organization estimates that by 2030 will die 8 million people annually due to consumption of tobacco, and 80% of them will occur in developing countries [2].
The literature reviewed shows that when taking into account the prevalence by education level, income, occupation and place of residence, tobacco consumption and related diseases affect disproportionately to people of low socioeconomic strata [3-5].
In Montevideo there are neighbourhoods, where live people of low socio-economic strata, whose prevalence is more than double, compared to other districts of the city [6].
A factor that may contribute to the tobacco consumption disparities is that quitting rates are different according to socioeconomic strata. Studies that have examined quitting rates in relation to smoker´ssocio-economic strata determined that the lower income or educational level less likely the smoker will succeed in quitting tobacco, and vice versa, that the higher education or income of people, the higher probability of success [7-9]. When a group of people has a higher prevalence of tobacco than average, interventions targeting these groups could reduce prevalence disparities [10-14].
Regarding intention to quit tobacco, there is no conclusive evidence about its relationship with the socio-economic strata. Studies in Australia, Canada and the United Kingdom [15] indicate that the higher the level of education or income more likely people will try to quit, but other works, also conducted in these countries and in the United States, not found such relationship [16,17].
The motivation to quit is an essential aspect for smoking cessation programs to achieve greater impact in reducing prevalence. Simple interventions that increase smoker´s motivation to quit could improve the cost-effectiveness of cessation programs.
This paper aims to evaluate the effectiveness of interventions that encourage smokers to quit tobacco, such as medical consultation and brief advice, controlling for socioeconomic and personal characteristics of those who intent to quit tobacco. Also it examines whether the intention of quitting is different depending on age tranches and if this is related to brief medical advice.
Materials and Methods
In Uruguay, Argentina y Brazil GATS is a national survey with urban and rural strata coverage. GATS was conducted as a household survey of people aged 15 years and older by the National Institute of Statistics of each country. In Uruguay an initial sample of 6558 households, completing 5591 individual interviews; in Argentina a sample of 9790 households carried out 6645 individual interviews and in Brazil the sample of 51011 households includes 39425 interviews [18-20].
A multi-stage cluster stratified sampling, designed to produce nationally representative data was used in all three cases. An individual was identified in each household randomly selected to participate in the survey. The response rate in households was 79.2%, 97.0% and 95.0%, the individual response rate was 93.8%, 98.5% and 98.9%, and the average response rate was 74.3%, 95.6 % and 94.0% in Argentina, Uruguay and Brazil respectively.
The dependent variable explained by the logit models is:
Intention to quit: Intent to quit smoking in the last 12 months, dichotomous categorical variable (0 do not try to quit, 1 try to quit).
The independent variables of logit models to estimate are [21-30]:
Age: Five dichotomous categorical variables are used, one for each tranche age, is 1 in each age tranche and 0 otherwise; the age tranches are up to 25 years old, between 26 y 35 years old, 36 and 45 years old, 46 and 59 years old, and 60 or more years old respectively.
Education: Three dichotomous categorical variables are used (Argentina and Uruguay), one for each education level, is 1 in the educational level and 0 otherwise; the categories are up to primary school, up to high school/technical school, up to university/high school teacher/technical school teacher respectively. In the case of Brazil four categorical variables are used, an additional variable is used for those without formal education.
Visit to the doctor: Visit to the doctor in the last 12 months. Dichotomous categorical variable, (0 do not visit to the doctor, 1 visit to the doctor).
Receive brief medical advice: Receive medical advice to quit, dichotomous categorical variable (0 do not receive brief medical advice, 1 receive brief medical advice).
Smoking frequency: Daily smoker or occasional smoker, dichotomous categorical variable (0 daily smokers, 1 occasional smoker).
Gender: Man or woman, dichotomous categorical variable (0 man, 1 woman).
Employment: Four categorical variables are used, one for each type of employment; the four types of employment are: government employee, private employee/self-employed, student (this category just to Uruguay and Argentina), housewife/retired/unemployed.
On the one hand, logit models are estimated to determine which personal characteristics and socio-economic have those who have tried quitting, and on the other hand, if medical interventions (medical consulting and brief medical advice) have an effect on those who have tried to quit tobacco. An analysis of variance (not reported) was performed to know if there are statistically significant differences among explanatory variables. After the ANOVA, binary logistic regression and odds ratios (relative risks) are estimated.
Results and Discussion
For each country the first logit is estimated using as an independent variable visit to the doctor in the last 12 months; the results are presented in Table 1.
Variables
Odds Ratio (OR)
Uruguay
Argentina
Brazil
Visited to the doctor
Received brief medical advice
Visited to the doctor
Received brief medical advice
Visited to the doctor
Received brief medical advice
Age (ref.<=25 years old)
26 a 35 years old
0,511***
0,358***
0.643*
0.573
1.026
0.834
36 a 45 years old
0.708
0,714
0.378**
0.335
0.776**
0.743
46 a 59 years old
0,538***
0,362***
0.702
0.697
0.800**
0.677**
60 years old and more
0,248***
0,192***
0.786
1.074
0.749**
0.620**
Education (ref. primary school/
without formal education(Brazil))
Primary school
---
---
---
---
1.447***
1.249
High school
0,776*
0,794
0.698
1.025
1.217*
1.002
University/Teacher
0,558***
0,416***
0.447***
0.670
0.929
0.887
Smoking frequency
(ref. daily smoker)
1,560**
2,356**
1.380
0.792
0.808*
1.123
Visited to the doctor
(ref. no visited to the doctor)
2,621***
---
0.839
---
1.666***
---
Received brief medical advice (ref. no received brief medical advice)
---
2,347***
---
0.983
---
1.274*
Gender
(ref. man)
0.821
1.041
1.063
1.849
1.159**
1.128
Employment (ref. government employee)
Private employee/self-employed
1.107
0.667
0,462*
0.599
0.856
1.003
Student
0.409
0.176**
0.596
1.395
---
---
Housewife/retired/unemployed
1.238
0.638
0.297***
0.483
0.794
0.924
Constant
0,853
2,516
3.323**
1.074
0.577***
1.009
Sample size
N=1394
N=545
N=1632
N=516
N=5026
N=2158
Statistical significance: 1%*** 5%** 10%*.
Table 1: Odds ratio estimates from logit models.
In all three countries, belonging to an older age group decreases the probability of try to quit compared to the reference group (25 years or less), however in Argentina the coefficients for the age tranches of 45 to 59 and 60 or more years old are not significant.
Having reached university in Uruguay and Argentina, as well as high school in Uruguay reduces the likelihood of trying to quit smoking compared to those with primary education. Having just primary school, or even high school in Brazil, increases the likelihood of quitting compared to those with no formal education.
Having visited the doctor in the last year increases the probability of intent to quit tobacco in Uruguay and Brazil, in Uruguay the respective OR increases 162.1% and in Brazil 66.6% compared to those who have not visited a doctor. In the case of Argentina this does not affect the probability of intent to quit.
In Uruguay being an occasional smoker increases the OR of intent to quit at 1.56 times but in Brazil the OR decreases 0.808 times regarding to those who smoke daily. In Argentina to be daily or occasional smoker is not a significant variable in relation to the intention of quitting.
In Uruguay and Argentina gender does not significantly influences the intention of quitting, although in Brazil being a woman increases the OR 15.9%.
Having visited the doctor in the last 12 months is a fact that could partly be determined by people´s health and partly due to his concern about his health. Therefore the results found for Uruguay and Brazil suggests that these two aspects or at least some of them could influence the intention to quit smoking; and that in Argentina these aspects would not influence in the intentions to quit.
In either of the two hypotheses about why the doctor attendance means that at least in Uruguay and Brazil health professionals would be in key position to encourage smoker´s intention to quit. In the second model estimated examines whether the brief physician advice is an act that helps people try to quit smoking.
A common result to the three countries is that the younger the smoker the more likely he will try to quit, and in Uruguay and Brazil this probability is even greater for those who have visited the doctor. Strikingly in Argentina visiting the doctor does not seem to affect the likelihood of thinking about quitting.
Those who visit the doctor in the last 12 months were asked if they had received brief advice to quit tobacco. For each country, a new model similar to the previous logit model was estimated by replacing the dependent variable visit to the doctor for the variable receive brief medical advice [31,32], (Table 1).
In this second model estimated, for those smokers who visited the doctor in last 12 months and received brief medical advice the OR increased 134.7% in Uruguay and 27.4% in Brazil, compared to those who did not receive such advice. Consistently with the result of the doctor's visit in Argentina, brief medical advice is not statistically significant to encourage quitting.
This suggests that in Uruguay and Brazil, but not in Argentina, brief medical advice is a very important medical intervention to encourage quitting smoking because it significantly changes the probability of try to quit among smokers who have visited a doctor in the last year.
Using the second model estimated, the probabilities of try to quit for people who have not received brief advice are calculated (Table 2). Then we simulated the probabilities of try to quit for those persons on the assumption if they had received brief medical advice(for Uruguay and Brazil).
Uruguay
Brazil
Age tranche
Without brief medical advice
If they had received brief medical advice
Without brief medical advice
If they had received brief medical advice
25 years old or less
53.6%
71.7%
50.9%
56.9%
26 to 35 years old
36.6%
56.8%
46.6%
52.7%
36 to 45 years old
53.7%
72.9%
44.4%
50.5%
45 to 59 years old
37.1%
57.8%
43.2%
49.1%
60 years old or more
25.8%
44.6%
41.5%
47.5%
Whole sample
42.4%
62.0%
45.4%
51.4%
Table 2: Probabilities of try quitting for smokers do not received brief medical advice.
At a general level, in Uruguay the impact of brief medical advice could be very important in people that have not received brief medical advice; the average probability of try to quit changes from 42.4% to 62.0%; while in Brazil the impact is moderate changing the probability from 45.4% to 51.4%.
In Uruguay the probability for people of 25 years old or less changes from 53.6% to 71.7%, and in the group between 36 and 45 years changes from 53.7% to 72.9%; implying that providing brief medical advice to young patients has a significant impact on the probability of try to quit (Table 2).
In Brazil the probability of the group of 25 years old or less increases from 50.9% to 56.9% and in the group between 26 and 35 years rises from 46.6% to 52.7%; hence the impact on the intention of quitting in young people is moderate.
Figure 1 shows that in general the percentage of visits to the doctor within the first four age ranges (from 15 to 59 years old) are lower compared to the rank of older (60 years old or older), which is expectable. However, there is some dispersion in the proportion of those who consult the doctor within the first four age ranges, ratios that are between 33.5% (Argentina, age range between 26 and 35 years old) and 62.5% (Brazil, age range between 46 and 59 years old).
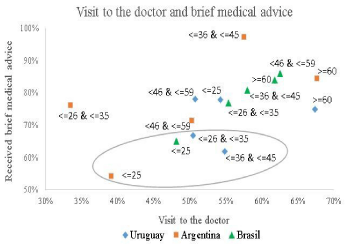
Figure 1: Visit to the doctor and brief medical advise.
There are four observations (Figure 1, inside the ellipse) corresponding to people in the youngest age tranches for the three countries, those with a percentage rate of receive brief medical advice below 67.0% and in lower proportion than other groups of age tranches.
When compared the three observations of Uruguay and Brazil that are inside the ellipse, with others of the same age tranche outside the ellipse, it is observed that the former receive proportionately less brief medical advice, although they have visited to the doctor in a similar or even in a lower percentage to the comparison groups.
Some young smokers who attend the doctor would be receiving less brief medical advice than the older. It is hypothesized that perhaps doctors do not consider smoking as a relevant issue regarding the motive of the consultation or due to the youth of the patient, despite the positive impact of brief medical advice to encourage the intention to quit tobacco in Uruguay and Brazil.
The medical brief advice rate for the age group between 46 to 59 years old is above 78% in Uruguay and Brazil and 71.5% in Argentina and on the age tranche of 60 years old or more is above 75 % in the three countries. It is argued that this may be because in this age tranche (46 and over) the motives for consultations may be mostly related to tobacco-related diseases, however the intention to quit in these groups is lower compared to younger age tranches. These data are consistent with international evidence which suggests that doctors practice more brief advice when the person is in older age tranches when prevalence of tobacco-related diseases is higher [33,34].
The above analysis shows that in all three countries there is room to improve medical intervention by increasing the proportion of brief medical advice on tranches of younger age, in Uruguay in people between 26 and 45 years old and in Argentina and Brazil in people up to 25 years old.
If medical advice is more likely according to the patient's age and eventually the reasons for consultation, it should be considered offering designed interventions for younger people, so that they could get some kind of advice or alternative medical intervention, even if the grounds for consultation are considered as unrelated to tobaccodiseases [35,36].
It is likely that younger people evaluate the risk of tobacco differently than an older person and in relative terms to other risks. The challenge is to develop an appropriate medical advice for individuals who often have a significant work-load with immediate concerns like stress or not have time for exercising, which should be part of a more holistic approach of health promotion and disease prevention.
This approach involves identify what may be the most relevant issues of concern to these young people. The literature related to intention to quit notes that overweight and aesthetics are important aspects in certain countries like the United States and the United Kingdom [37] as well as the status of smoker husband [38], gender, age, educational level, age of onset of smoking, smoking intensity [39], and other cultural aspects [40].
Regarding the intention to quit, can be seen (Figure 2) that there is a central mass of observations with intention to quit rates between 39.5% and 44.2% (in the ellipse of the medium), without a significant statistical difference among them, that correspond almost entirely to the first four age ranges (from 15 to 59 years old). The intention to quit in Uruguay and Brazil in the group of 60 years old or more is lower than this core set of observations.
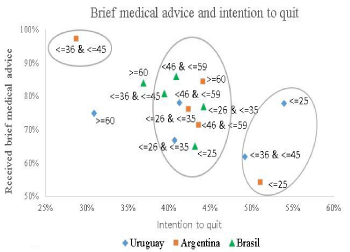
Figure 2: Brief medical advise and intention to quit.
In Brazil the intention to quit in the first four age groups is concentrated in the central ellipse with values that are not statistically different.
In Argentina and Uruguay it is observed a greater dispersion of the intention to quit in the first four age groups, with three age tranches whose percentage rate of intention to quit is greater than the core group. Of these three cases two correspond to the group of up to 25 years in Argentina and Uruguay and the third is the group between 36 and 45 years in Uruguay. This higher intention to quit in young individuals cannot be explained only by brief medical advice, because they receive brief medical advice in equal or lower proportion than the average of the other groups.
An alternative explanation is that in Uruguay and Argentina (maybe also in Brazil) tobacco control policies have encouraged quitting through pictograms in cigarettes packs, smoke free public, and in Uruguay due to higher tobacco taxes and ban on advertising, promotion and sponsorship of tobacco products.
Conclusions
The present study confirms that medical consultation and brief medical advice to quit tobacco use are effective to encourage quitting in Argentina, Brazil and Uruguay.
However, it should work for young people that attend to the doctor receive brief medical advice, at least, in similar proportions like people in other age tranches. Brief advice should be tailored to the needs and characteristics of this population and form part of a comprehensive strategy for health promotion and disease prevention.
This strategy should include addressing threats and concerns to the health of young people like overweight, alcohol consumption, stress and anxiety management, etc., that help and encourage them to develop a healthier lifestyle.
This comprehensive approach could enhance cost-effectiveness of medical interventions because they are people who are mostly healthy, with larger healthy years to gain. Therefore the health gain could be bigger with a higher impact in order to reduce direct and indirect costs of tobacco epidemic.
Furthermore health programs designed for youth with a comprehensive approach that help to manage or avoid other risks besides tobacco, could imply a gain in cost-effectiveness of such comprehensive programs because are increased the risks quantity that are prevented.
Strikingly in Uruguay and Argentina we find that intention to quit is greater in smokers of low socioeconomic strata, which contrasts with some evidence for developed countries. This implies that in these two countries disparities generated by tobacco consumption could be reduced if it is achieved that the intentions of quitting become into effective quit attempts. This finding implies that current national programs of cessation are an important tool to encourage quitting, and should be strengthened and focused on smokers of low socioeconomic strata and youth.
In Brazil the intention of quitting is higher in groups with up to primary or high school in relation to those without formal education, so that specific interventions should be developed on the latter to reduce the disparity in tobacco consumption.
Additionally, reduce tobacco use disparities requires apply a set of tobacco control measures which reach great masses of the population with low education and income; this especially means to decrease the affordability of tobacco products, through increased of tobacco taxes and reducing the availability of illegal cigarettes which are mainly consumed by these social groups.
More research is needed to determine the reasons why the intention of quitting is higher in groups of young people in the three countries, and know what aspects concern to this group of people for the purpose of developing appropriate and effective interventions. Especially discriminate the weight given by them to risks with more immediate effects in relation to risks with effects of longer term as smoking or not exercising.
Acknowledgements
The authors acknowledge the financial support of the School of Business at the University Adolfo Ibañez and the American Cancer Society to carry out this research; and to Guillermo Paraje and Adriana Blanco for his helpful comments that allowed improving this article.
References
- World Health Organization. World health report 2003. Geneva, World Health Organization. 2003.
- Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med. 2006; 3: e442.
- Bobak M, Jha P, Nguyen S, & Jarvis M. Poverty and smoking. P Jha and FJ Chaloupka editors, in tobacco control in developing countries. New York: Oxford University Press. 2000; 41-61.
- Giskes K, Kunst AE, Benach J, Borrell C, Costa G, Dahl E, et al. Trends in smoking behaviour between 1985 and 2000 in nine European countries by education. J Epidemiol Community Health. 2005; 59: 395-401.
- Harper S & Lynch J. Trends in socioeconomic inequalities in adult health behaviors among US states, 1990–2004. Public Health Reports. 2007; 122: 177-189.
- Curti D. Los impuestos al tabaco como una estrategia de salud pública. Centro para la Investigación de la Epidemia del Tabaquismo. Mimeo. 2015; 1-18.
- Kotz D, West R. Explaining the social gradient in smoking cessation: it's not in the trying, but in the succeeding. Tob Control. 2009; 18: 43-46.
- Schaap MM, Kunst AE. Monitoring of socio-economic inequalities in smoking: learning from the experiences of recent scientific studies. Public Health. 2009; 123: 103-109.
- JL Reid, D Hammond, C Boudreau, GT Fong, M Siahpush. Socioeconomic disparities in quit intentions, quit attempts, and smoking abstinence among smokers in four western countries: Findings from Tobacco Control Four Country Survey Nicotine & Tobacco Research. 2010; 12: S20-S33.
- Borland R, Hyland A, Cummings KM, Fong GT. One size does not fit all when it comes to smoking cessation: observations from the International Tobacco Control Policy Evaluation Project. Nicotine & Tobacco Research. 2010; 12: S1–S3.
- Sarkar BK, Arora M, Gupta VK, Reddy KS. Determinants of tobacco cessation behaviour among smokers and smokeless tobacco users in the states of Gujarat and Andhra Pradesh, India. Asian Pacific Journal of Cancer Prevention. 2013; 14: 1931-1935.
- Fleischer NL, Thrasher FL, Sáenz de Miera Juárez B, Reynales-Shigematsu LM, Arillo-Santillán E, Osman A, et al. Neighbourhood deprivation and smoking and quit behaviour among smokers in Mexico: findings from the ITC Mexico Survey. Tobacco Control. 2015; 24: 56-63.
- Kadowaki T, Okamura T, Funakoshi T, Okayama A, Kanda H, Miyamatsu N, et al. Effectiveness of annual interventions for smoking cessation in an occupational setting in Japan. Environmental Health and Preventive Medicine. 2004; 9: 161–164.
- Hu TW, Lin Z, Keeler TE. Teenage smoking, attempts to quit, and school performance. Am J Public Health. 1998; 88: 940-943.
- Siahpush M, McNeill A, Borland R, Fong GT. Socioeconomic variations in nicotine dependence, self efficacy, and intention to quit across four countries: Findings from the International Tobacco Control (ITC) Four Country Survey. Tobacco Control. 2006; 15: 71-75.
- Reid JL, Hammond D, Driezen P. Socio-economic status and smoking in Canada, 1999-2006: has there been any progress on disparities in tobacco use? Can J Public Health. 2010; 101: 73-78.
- Hyland A, Borland R, Li Q, Yong HH, McNeill A, Fong GT, et al. Individual-level predictors of cessation behaviours among participants in the International Tobacco Control (ITC) Four Country Survey. Tobacco Control. 2006; 15: 83-94.
- Ministerio de Salud, Uruguay; Organización Panamericana de la Salud - Organización Mundial de la Salud. Encuesta Mundial de Tabaco en Adultos 2009. Uruguay, 2009.
- Ministero de Salud, Argentina; Organización Panamericana de la Salud - Organización Mundial de la Salud. Encuesta Mundial de Tabaquismo en Adultos (EMTA). Argentina, 2012.
- Ministerio da Saúde, Brasil; Instituto Nacional de Cancer; Organización Panamericana de la Salud – Organización Mundial de la Salud. Encuesta Mundial de Tabaco en Adultos (EMTA). Brazil, 2010.
- Rajmohan P, Venkatesan S, Persai D, Trivedi M, and Mathur MR. Factors determining intention to quit tobacco: exploring patient responses visiting public health facilities in India. Tobacco Induced Diseases. 2014; 12: 1.
- Diemert LM, Bondy SJ, Brown KS, Manske S. Young adult smoking cessation: predictors of quit attempts and abstinence. Am J Public Health. 2013; 103: 449-453.
- Breslau N, Peterson EL. Smoking cessation in young adults: age at initiation of cigarette smoking and other suspected influences. Am J Public Health. 1996; 86: 214-220.
- Rosendo I, Fonseca G, Guedes AR, Martins V. Characterisation of smokers and factors influencing motivation to stop smoking Revista Portuguesa de Pneumología. 2009; 15: 783-802.
- Coambs RB, Li S, Kozlowski LT. Age interacts with heaviness of smoking in predicting success in cessation of smoking. Am J Epidemiol. 1992; 135: 240-246.
- Ramon Torrell JM, Bruguera Cortada E, Fernández Pinilla C, Sanz de Burgoa V, Ramírez Vázquez E. [Reasons for smoking cessation in Spain by gender and age]. Gac Sanit. 2009; 23: 539.
- Khuder SA, Dayal HH, Mutgi AB. Age at smoking onset and its effect on smoking cessation. Addict Behav. 1999; 24: 673-677.
- MacyJ T, Seo D, Chassin L, Presson CC. Prospective predictors of long-term abstinence versus relapse among smokers who quit as young adults. Journal of Public Health. 2007; 97: 1470-1475.
- Clark MA, Rakowski W, Kviz FJ, Hogan JW. Age and stage of readiness for smoking cessation. Journal of Gerontology. 1997; 52: S2I2-S22I.
- Li L, Borland R, Yong H, Fong GT, Bansal-Travers M, Quah ACK, et al. Predictors of smoking cessation among adult smokers in Malaysia and Thailand: findings from the International Tobacco Control Southeast Asia Survey. Nicotine & Tobacco Research. 2010; 12: S34-S44.
- Buckland A, Connolly MJ. Age-related differences in smoking cessation advice and support given to patients hospitalised with smoking-related illness. Age Ageing. 2005; 34: 639-642.
- Young JM, Ward JE. Influence of physician and patient gender on provision of smoking cessation advice in general practice. Tobacco Control. 1998; 7: 360–363.
- Maguire CP, Ryan J, Kelly A, O'Neill D, Coakley D, Walsh JB. Do patient age and medical condition influence medical advice to stop smoking? Age Ageing. 2000; 29: 264-266.
- Chang F, Hu T, Lo S, Yu P, Chao K, Hsiao M. Quit smoking advice from health professionals in Taiwan: the role of funding policy and smoker socioeconomic status. Tobacco Control. 2010; 19: 44-49.
- Aveyard P, Raw M. Improving smoking cessation approaches at the individual level. Tob Control. 2012; 21: 252-257.
- Melvin CL, Dolan-Mullen P, Windsor RA, Whiteside HP Jr, Goldenberg RL. Recommended cessation counselling for pregnant women who smoke: a review of the evidence. Tob Control. 2000; 9 Suppl 3: III80-84.
- Shang C, Chaloupka FJ, Fong GT, Thompson M, Siahpush M, Ridgeway W. Weight control belief and its impact on the effectiveness of tobacco control policies on quit attempts: findings from the ITC 4 Country Project. Tobacco Control. 2015; 0: 1-7.
- Rüge J, Ulbricht S, Schumann A, Rumpf HJ, John U, Meyer C. Intention to quit smoking: is the partner’s smoking status associated with the smoker’s intention to quit? International Journal of Behavioral Medicine. 2008; 15: 328-335.
- Curry SJ, Sporer AK, Pugach O, Campbell RT, Emery S. Use of tobacco cessation treatments among young adult smokers: 2005 National Health Interview Survey. Am J Public Health. 2007; 97: 1464-1469.
- Woodruff SI, Talavera GA, Elder JP. Evaluation of a culturally appropriate smoking cessation intervention for Latinos. Tob Control. 2002; 11: 361-367.
