Case Report
Austin J Dermatolog. 2014;1(4): 1018.
Successful Treatment of Morphea with Narrowband UVB (310-315 nm)-Case Report
Anca Chiriac1*, Piotr Brzezinski2, Tudor Pinteala4, Anca E Chiriac4, Caius Solovan3 and Liliana Foia4
1Department of Dermatology, University Apollonia, Iasi-Romania
2Department of Dermatology, 6th Military Support Unit, Poland
3University of Medicine and Pharmacy "V Babes" Timisoara-Romania
4University of Medicine and Pharmacy "Gr T Popa" Iasi, Romania
*Corresponding author: Anca Chiriac MD, PhD, Department of Dermatology, University Apollonia, Iasi-Romania
Received: July 28, 2014; Accepted: August 22, 2014; Published: August 26, 2014
Abstract
Morphea is very difficult to treat because of it being recalcitrant to variable therapeutical attempts. A 64 year-old woman, diagnosed on clinical and histological findings with localized morphea, was treated with narrowband UVB and emollients with favorable outcome. Objectively, post-treatment, the plaque was less indurated, softer to palpation, and less hyperpigmented; skin thickness was measured by using high-frequency ultrasound technique(18 MHz) proving a decreased of dermal thickness from 0.4cm to 0.25 cm within 4 months of therapy. Therefore, this treatment procedure could be an option in managing morphea.
Case Presentation
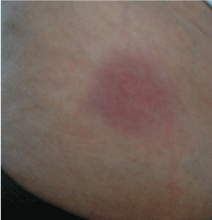
A 64 year-old Caucasian woman was diagnosed 6 months ago with localized scleroderma en plaque (morphea) on the right side of abdominal wall. Clinical examinations observed a violaceous round-oval sclerotic plaque over the right side of abdominal wall; the plaque proved to be indurated on palpation (Figure 1). A skin biopsy revealed interstitial inflammation and homogenization of collagen bundles in the dermis and subcutis.
Figure 1: Violaceous round-oval sclerotic plaque over the right side of abdominal wall.
The patient's medical history included arterial hypertension, well controlled by low-dose combination of perindopril arginine with indapamide.
X-ray showed no pulmonary involvement; electrocardiographic record and echocardiogram were reported as normal; renal function and urine analysis within normal limits; no hepatic dysfunction; leukocytes count with normal hemoglobin and differential count; C3, C4, rheumatoid factor, Scl70, lupic anticoagulant, ANAs, Anti DNA, antineutrophil cytoplasmic antibodies (ANCAS), anticardiolipins, anti-Ro, anti-La, anti-Sm, anti-RNP 4.8 all within standard values. Abdominal ultrasonography showed no pathological findings, serologic screening for Borrelia burgdorferi, hepatitis virus B and C were negative, and thyroid function was normal. No favorable results were described after the use of potent topical steroids administered continuously for several months.
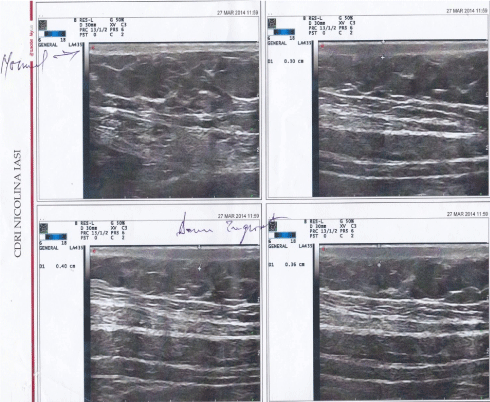
Cutaneous ultrasonography was performed and skin thickness was measured by using high-frequency US (18 MHz): dermal thickness was 0.4cm in its highest point (Figure 2).
Figure 2: Cutaneous ultrasonography before narrow-band UVB; dermal thickness was 0.4cm in its highest point.
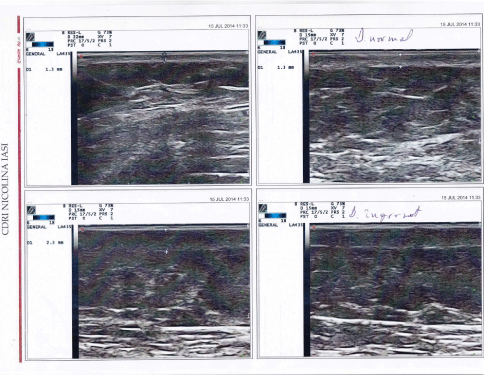
Narrowband UVB (310-315 nm) was started for the following months accompanied by emollients, with favorable results: softer skin on palpation. New measurements of skin thickness were performed using ultrasonography and revealed the reduction of dermal thickness to 0.25cm (Figure 3).
Figure 3: Cutaneous ultrasonography after narrow band UVB; highest thickness is 2.5mm (0.25cm).
Discussion
For a long period of time solar ultraviolet (UV) radiation (heliotherapy) along with phototherapy has been used in order to attempt treating several skin diseases [1]. Nowadays, phototherapy is a valuable therapeutic method in numerous skin diseases: psoriasis, atopic dermatitis, vitiligo, morphea, and mycosis fungoides [2].
UVA-1 has been reported to be effective in morphea based on reducing the number of Langerhans cells and mast cells [3]. Recently, UVB phototherapy has been tested in treating morphea, showing good results in association with acitretin [4] or antimalarials [5].
UVB radiation reaches the epidermis and the upper dermis [5], while UVA radiation penetrates more deeply into the dermis; with effects on blood vessels, dendritic cells, fibroblasts, mast cells, granulocytes [6] Narrowband UVB causes local and systemic immunosuppressive effects by activating keratinocytes, circulating and cutaneous T lymphocytes, monocytes, Langerhans cell, mast cells and fibroblasts [7,8].
UVB radiation is absorbed by endogenous chromophores (nuclear DNA) with the formation of DNA photoproducts and ultimately suppression of DNA synthesis [8]. Immune suppression is achieved also by synthesis of prostaglandins and cytokines by UV radiation [8].
The immunomodulatory effects of UVB radiation can explain, at least in part, the beneficial effects observed in morphea.
References
- Roelandts R. The history of phototherapy: something new under the sun? J Am Acad Dermatol. 2002; 46: 926-930.
- Walker D, Jacobe H. Phototherapy in the age of biologics. Semin Cutan Med Surg. 2011; 30: 190-198.
- Kroft EB, Berkhof NJ, van de Kerkhof PC, Gerritsen RM, de Jong EM. Ultraviolet A phototherapy for sclerotic skin diseases: a systematic review. J Am Acad Dermatol. 2008; 59: 1017-1030.
- Newland K, Marshman G. Success treatment of post-irradiation morphoea with acitretin and narrowband UVB. Australas J Dermatol. 2012; 53: 136-138.
- Brownell I, Soter NA, Franks AG Jr. Familial linear scleroderma (en coup de sabre) responsive to antimalarials and narrowband ultraviolet B therapy. Dermatol Online J. 2007; 13: 11.
- Pavel S. Light therapy (with UVA-1) for SLE patients: is it a good or bad idea? Rheumatology (Oxford). 2006; 45: 653-655.
- Juzeniene A, Moan J. Beneficial effects of UV radiation other than via vitamin D production. Dermatoendocrinol. 2012; 4: 109-117.
- Bulat V, Situm M, Dediol I, LjubiciÄ I, BradiÄ L. The mechanisms of action of phototherapy in the treatment of the most common dermatoses. Coll Antropol. 2011; 35: 147-151.