Abstract
Backwards planning in dental implantology helps to achieve optimal prosthetic results. For implant surgery in the mandible highest patient-safety is necessary. Therefore, in the radiological image of the mandible the nerve position must be clearly defined. Changes of the nerve position caused by cysts or after trauma can lead to different treatment planning or might result in unexpected complications especially during implant surgery. This article critically discusses the decision tree and risk assessment and shows a clinical case where nerve detection was not possible.
Keywords: Alveolar nerve; Cone beam CT; Decision tree; Risk assessment; Short implants; Nerve disposition; Piezo surgery; Minimal invasive implantology
Abbreviations
IAN: Inferior Alveolar Nerve; CT: Computed Tomography; CBCT: Cone Beam CT; -: no; +: yes
Introduction
The complex and advanced developments in dental implantology and guided surgery maintain high success rates. According to numerous studies, if implants are inserted and restored by today’s standards, the success rate is about 95% over ten years [1]. The incidents of periimplantitis and implant failures under these conditions are less than 5% [2]. If clinical relevant risk factors or misdiagnosis occurs, this results in significant lower success rates [3].
None the less complications such as implant loss, technical complications or nerve damage can occur [4]. Especially in the mandibular molar region individual anatomical structures of every patient may vary [5]. This might become a major challenge in treatment planning. Irritation of the inferior alveolar nerve after surgical treatment such as wisdom tooth osteotomies is often described [6]. These irritation phenomena are observed in non-surgical endodontic in rare cases. The following reasons for nerve irritations are given: The most common cause is, according to a summary of an article by Knowles, the overfilled root filling material in the nerve canal within the framework of an endodontic treatment [7]. As a consequence, a paresthesia up to a complete loss of sensitivity is reported, or pain was only mentioned in very few cases [8,9]. Caused by an infection a sensibility disturbance can occur due to a displacement of infectious materials or chemicals [10]. This can be treated surgically or with appropriate medication. A similar phenomenon is known as the Vincent-Symptom. After a block anesthesia on the Inferior Alveolar Nerve (IAN), due to toxic or physical damage a mostly reversible nerve irritation can occur [11, 12]. Seldom reported, as in the article by Krogstad et al. (1997), is a paresthesia after orthodontic treatments displacement of teeth causing close contact with the IAN [13].
Besides the postoperative wound infection, damage to the inferior alveolar nerve plays a significant role. Complications and healing intervals are dependent on the age of the patient and rise significantly in patients over 25 years of age [14].
An IAN channel has a large variance in its position. It is located from 4.9 mm to 17.4 mm from the buccal side and runs precise on the high-level cortical surface of the mandible. The buccal tongue IAN canal position is influenced by age and race. On the average, older and white patients have a shorter gap between the buccal side of the canal and the tongue-side of the mandible border. To reduce the risk of an IAN injury, these variables must be taken into consideration when planning a mandible osteotomies or using monocortical plates [15].
Nerve displacement correlating to mandibular cysts
Solitary bone cysts mostly arise in the second decade of people’s lives, and men and women are equally affected [16]. Solitary cysts usually occur exclusively in the lower jaw, and are mainly located in the corpus and the symphysis.
In general, solitary bone cysts are lesions displaying no clinical symptoms. They are usually discovered by accident during routine radiological examinations. The clinical findings are generally vestibular situated swellings, rarely causing pain or paraesthesia of the lips [17].
Radiological findings in cysts are a sharp, restricted, roundish or osteolytic with a partial sclerotic edge. Often there is an interdental, to be precise, an intraradicular, expanse which is described as scalloped in shape. In accordance with the radiological findings, which barely ever show signs of resorption of the apex or nerve resorption patients rarely complain of pain or paresthesia. In these cases, the nerve is displaced by the cyst without resorption or destruction. Other factors such as orthognathic surgery or a trauma can result in a nerve disposition [18]. Even when the common therapy like a careful removal of the fibrous heath of the cavity, and to induced bleeding for a bony consolidation is performed, the nerve will not reposition.
As nerve disposition, due to cysts might occur dental implant treatment planning can be challenging. Due to this fact, the changing courses of nerve tracts in the oral cavity can lead to unexpected complications especially during implant surgery.
As patients are statistically getting older and having lower bone remodeling rates as well as lower general health status, new techniques for dental implant treatments are necessary. This nowadays leads to increasingly shorter implants being inserted to avoid augmentation procedures. Short implants are discussed critically in literature. Overall the failure rate of long implants compared to short implants is the same when the loading axis was taken into account [19]. The use of short implants in cases where nerve detection is radiologically not feasible has not been described yet. Therefore, the decision-making process of cases with undetectable alveolar nerve was described and a corresponding case report is presented.
Case Presentation
A 49 years old patient presented at the dental clinic Danube Private University (DPU) in Austria, with a referral from her dentist, and requested implants at the missing teeth 36 and 46.
As an anatomical abnormality a post-traumatic displacement of the inferior alveolar nerve after an accident in 1987 was presumable. Further medical history showed a diagnosed fibromyalgia and minimal regular consumption of alcoholic beverages. The patient is a smoker and suffers occasional bouts of claustrophobia. She regularly takes the prescribed medication Pregamid (GL pharma, Austria) in order to cope with and control the sudden claustrophobic attacks. The patient showed no signs of paresthesia in the left and right lower jaw preoperatively.
Clinically the first molars (36 and 46) were missing in the lower jaw. In a standard Orthopantomography (OPG) the alveolar nerve in the left jaw was undetectable (Figure 1).
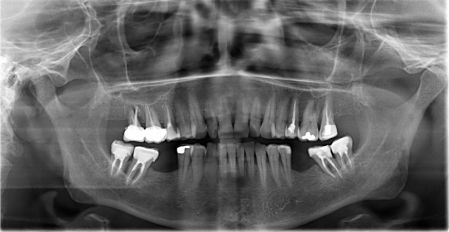
Figure 1: Orthopantomography showing undetectable alveolar nerve position
region 36.
A cone beam CT was performed additionally (Figure 2) for further detection of the alveolar nerve position. Even in the cone beam CT the nerve position in this case was not clearly detectable.
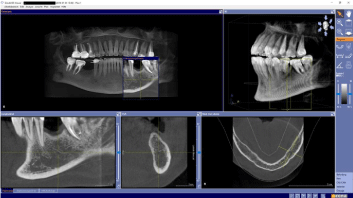
Figure 2: Cone beam CT screenshot regio 36 in all axis with regular compact
bone and undetectable alveolar nerve position.
In the lower jaw, the 1st molars on both sides were missing (Figure 3). A therapy plan was established, shown to the patient and clearly explained. Pre-operative discussions, concerning the risks and possible complications, were held and documented carefully. The patient still decided to have an implant surgery for reconstruction of both molars.
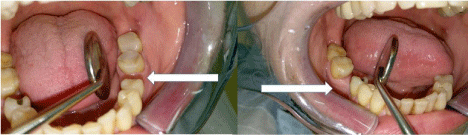
Figure 3: Intraoral site with missing first molars (regio 36 and 46, arrow) prior
to implant placement.
For guided surgery the plaster model was scanned (3 Shape scanner Modell NEW D850, Copenhagen, Denmark). The digital implant planning was carried using CoDiagnostix (Dental wings, 2251 Letourneux, Montreal, Canada) and a drill guide was 3D printed afterwards (3D Printer Varseo, Bego Bremen)(Figure 4-7)
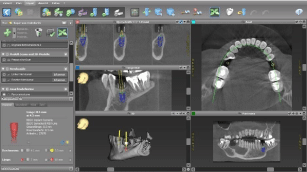
Figure 4: Screenshot (Co Diagnotix, Dental Wings, Canada) of the treatment
planning for implant position.
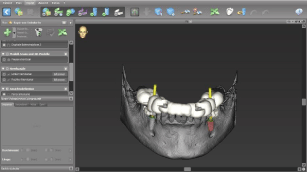
Figure 5: Screenshot of digital dental implant treatment planning using a
surgical guide.
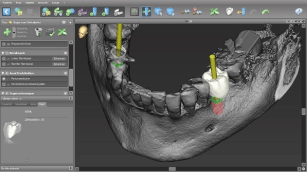
Figure 6: Backwards planning for an optimal implant position and axial
loading of the implant.
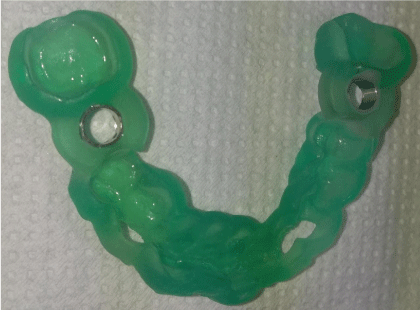
Figure 7: 3D printed surgical guide (Varseo, BEGO, Bremen, Germany) with
drill sleeves.
Treatment
After local anaesthesia a centric bleeding point through the drill guide was marked and a full flap with release incisions was elevated using piezoelectric devices (PR1, Mectron, Italy). After bone exposure the depth drill as well as the enlarging drills with the surgical guides was used. The implant bed was prepared two millimetres short of the implant length using conventional drills. For full length preparation a piezoelectric device was used (OT9, Mectron, Italy) up to 8.5mm length (Figure 8).
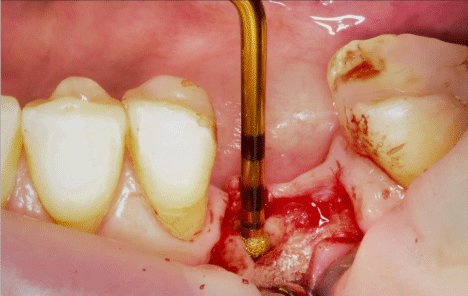
Figure 8: Intraoperative site with piezoelectric device (OT9, Mectron, Italy)
for implant bed preparation.
Since a very porous bone structure was present apically the thread was cut by hand only in the compact bone. The angulation and depth were carefully controlled using parallel pins. Now the Bego RSX implant with a diameter of 4.1mm and length of 8.5mm was inserted. The cover screw was inserted and the bone chips from the drills were collected and augmented buccal. Wound closure was performed with sutures.
In region 46 a conventional surgical procedure was performed and an implant (length 10mm, diameter 4.1mm, RSX, BEGO; Germany) was inserted. For postoperative controls an x-ray (orthopantomography) was performed (Figure 9). Postoperative prescription of Augmentin (Smith Kline Beecham Pharmaceuticals, Worthing, Great Britain) was indicated. The postoperative control after two days showed no signs of paresthesia or dysfunctions.
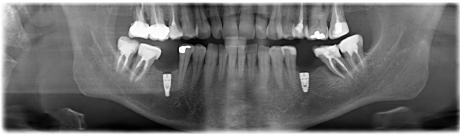
Figure 9: Postoperative orthopantomography with inserted dental implants.
Discussion
The case presented shows an implant treatment case where the alveolar nerve was not detectable after a trauma. In cases with nerve disposition careful consideration for implantological treatment is necessary to avoid major complications.
When a secure detection of the alveolar nerve is not possible alternative treatment options should be discussed. One alternative is to use even shorter implants. However, these have a limited medical indication, and in the molar region, these should not be seen as the ideal prime choice [20]. Short implants nevertheless have become an alternative to bone augmentation in dental implantology. Design of shorter implants and longer observation times are current research issues [21]. When 8mm implants are used in the mandible, it has been discovered that they have a similar survival rate as longer implants. Here the implant-crown ratio as well as the loading axis of the implant has to be evaluated carefully for long term survival [22]. In these cases the use of surgical guides and backwards planning has shown favorable outcomes compared to free hand drilling [23].
A further alternative is the possibility of the vertical augmentation with autologous bone or allogenic materials. A controversial discussion would arise, however, regarding the long term prognosis as a consequence of the re-absorption rate, which is up to 30% after five years [24].
Furthermore, this method with autologous augmentation is only just possible in the cases where crestal bone is atrophied and donor site is limited though. This would in addition, implement to create a second donor site by using bone material from other regions such as the retromolar zone or the iliac crest. The rate of long-term medical complaints in this area is 16.5% and has thus a strong influence on the patient’s acceptance for iliac donor site [25].
An alternative treatment would be a prosthetic restauration with a bridge from tooth 35 to tooth 37. This alternative can be considered if the neighboring teeth are in good condition and suitable.
Piezoelectric surgical techniques
Protecting the inferior alveolar nerve is the highest priority; in addition, the patient should be given the best possible medical care with the highest level of safety. Piezosurgery is a relatively new technique for osteotomy and osteoplasty that utilizes ultrasonic vibration. The piezosurgery device is essentially an ultrasound machine with modulated frequency and a controlled tip vibration range. The ultrasonic frequency is modulated from 10,30, and 60 cycles/s (Hz) to 29 kHz. The low frequency enables cutting of mineralized structures but not soft tissue. Power can be adjusted from 2.8 to 16 W, with preset power settings for various types of bone density and applications. The piezosurgery tip vibrates within a range of 60-210μm, which allows clean cutting with precise incisions [26]. Piezosurgical techniques can be used for different applications such as retrograde preparation of root canals. It performs bone cutting with great precision facilitating ridge augmentation and ridge expansion, tooth extraction, ankylotic tooth osteomie and surgical orthodontic surgeries [27]. In the presented case it was used for the implant bed preparation in close vicinity to the possible position of the alveolar nerve. Piezoelectric surgery is a method which is also suitable for surgical nerve transposition [28]. As an alternative it would have been to set implants in the mandible after lateralization of the alveolar nerve. This is to prepare the nerve from the mental foramen distally and secure the nerve by transposition while implant bed preparation is performed as described by Bovi [29]. This implements stability loss in the mandible and might result in mandibular fracture [30].
An important risk in the nerve transposition treatment in the mandible is a temporary or permanent irritation of the nerve, which can result in paresthesia. Various studies dealt with this risk: In 1992, Rosenquist stated that of 26 implants which were examined [31], 10% of the patients had no sensory disorders after twelve months. According to Kan, the rate of sensory disorders after surgical manipulation was 77.8% whereas the patients where no surgical transposition was performed was 33.3% [32]. The study furthermore compared deposition of the foramen or the alveolar nerve. Here 21 operations with 64 implants after a time span of 10-67 months were investigated. He discovered that there were a higher proportion of sensory disturbances in the deposition of the foramina as compared to the deposition of the IAN.
After surgery, the patient showed no paresthesia or other nerve irritations in the left lower jaw. This was investigated using simple techniques such as two point discrimination and sensitivity test which are very reliable and easy to perform in everyday practice [33]. Only when these tests show negative results further neurological investigations can become necessary.
In the presented case the standard radiological examination prior to implant placement was performed. As the panoramic x-ray technique gives a very good overview and thus became the standard radiographic image in dentistry the evaluation and the detection of the alveolar nerve can be difficult [34]. In these cases, an additional three dimensional radiographic techniques can be helpful. Here the CBCT often helps to identify the alveolar nerve canal and enable sufficient treatment planning [35].
In conclusion, there is a defined individual clinical decision guide for patients necessary, where the alveolar nerve is not clearly detectable (Figure 10).
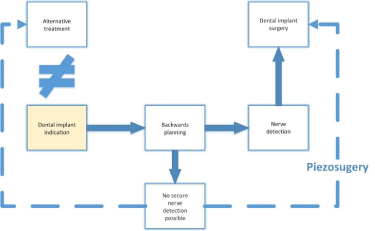
Figure 10: Decision Tree for implant treatment in correlation to nerve
detection.
Units
- Radiological support
- OPTG
- CBCT (Cone Beam CT) with a reference pattern and reference bowls
- Plaster Model
- Bego RSX Line guided surgery
- Piezo
- 3 Shape scanner, Modell NEW D850
- Program Dental Wings Inc.
- CoDiagnostix
- 3D Printer Varseo, Bego Bremen
Supplementary
Further treatment: A temporary Cerec crown proved to be an ideal interim solution in guaranteeing the patient the closure of the tooth gaps as quickly as possible.
After a three-month healing period, the patient will be supplied with 2 prosthetic VMK crowns by her dentist. The medical indication for two single crowns is given and is the ideal individual form of treatment in this case.
References
- Papaspyridakos P, Chen CJ, Chuang SK, Weber HP, Gallucci GO. A systematic review of biologic and technical complications with fixed implant rehabilitations for edentulous patients. Int J Oral Maxillofac Implants. 2012; 27: 102-110.
- Ramanauskaite A, Baseviciene N, Wang HL, Tözüm TF. Effect of history of periodontitis on implant success: meta-analysis and systematic review. Implant Dent. 2014; 23: 687-696.
- Roos-Jansåker AM, Renvert H, Lindahl C, Renvert S. Nine- to fourteen-year follow-up of implant treatment. Part III: factors associated with peri-implant lesions. J Clin Periodontol. 2006; 33: 296-301.
- Lee JH, Lee JB, Park JI, Choi SH, Kim YT. Mechanical Complication Rates and Optimal Horizontal Distance of the Most Distally Positioned Implant-Supported Single Crowns in the Posterior Region: A Study with a Mean Follow-Up of 3 Years. J Prosthodont. 2015.
- Kim ST, Hu KS, Song WC, Kang MK, Park HD, Kim HJ. Location of the mandibular canal and the topography of its neurovascular structures. J Craniofac Surg. 2009; 20: 936-939.
- Gulicher D, Gerlach KL. [Incidence, risk factors and follow-up of sensation disorders after surgical wisdom tooth removal. Study of 1,106 cases]. Mund Kiefer Gesichtschir. 2000; 4: 99-104.
- Knowles KI, Jergenson MA, Howard JH. Paresthesia associated with endodontic treatment of mandibular premolars. J Endod. 2003; 29: 768-770.
- Grötz KA, Al-Nawas B, de Aguiar EG, Schulz A, Wagner W. Treatment of injuries to the inferior alveolar nerve after endodontic procedures. Clin Oral Investig. 1998; 2: 73-76.
- Giuliani M, Lajolo C, Deli G, Silveri C. Inferior alveolar nerve paresthesia caused by endodontic pathosis: a case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001; 92: 670-674.
- Coskunses FM, Sinanoglu A, Helvacioglu-Yigit D, Abbott PV. The extrusion of root canal cement containing paraformaldehyde into the inferior alveolar nerve canal resulting in infection and numbness. Int Endod J. 2015.
- Pogrel MA, Thamby S. Permanent nerve involvement resulting from inferior alveolar nerve blocks. J Am Dent Assoc. 2000; 131: 901-907.
- Pogrel MA. Permanent nerve damage from inferior alveolar nerve blocks: a current update. J Calif Dent Assoc. 2012; 40: 795-797.
- Krogstad O, Omland G. Temporary paresthesia of the lower lip: a complication of orthodontic treatment. A case report. Br J Orthod. 1997; 24: 13-15.
- Chiapasco M, Crescentini M, Romanoni G. Germectomy or delayed removal of mandibular impacted third molars: the relationship between age and incidence of complications. J Oral Maxillofac Surg. 1995; 53: 418-422.
- Greenstein G, Tarnow D. The mental foramen and nerve: clinical and anatomical factors related to dental implant placement: a literature review. J Periodontol. 2006; 77: 1933-1943.
- BARNES R. Aneurysmal bone cyst. J Bone Joint Surg Br. 1956; 38-38B: 301-311.
- Struthers PJ, Shear M. Aneurysmal bone cyst of the jaws. (I). Clinicopathological features. Int J Oral Surg. 1984; 13: 85-91.
- Rich J, B.A. Golden, and C. Phillips. Systematic review of preoperative mandibular canal position as it relates to postoperative neurosensory disturbance following the sagittal split ramus osteotomy. Int J Oral Maxillofac Surg. 2014; 43: 1076-1081.
- Monje A, Chan HL, Fu JH, Suarez F, Galindo-Moreno P, Wang HL. Are short dental implants (<10 mm) effective? a meta-analysis on prospective clinical trials. J Periodontol. 2013; 84: 895-904.
- Wehrbein H, Yildirim M, Diedrich P, Osteodynamics around orthodontically loaded short maxillary implants. J Orofac Orthop. 1999. 60: 409-415.
- Felice P, Cannizzaro G, Barausse C, Pistilli R, Esposito M. Short implants versus longer implants in vertically augmented posterior mandibles: a randomised controlled trial with 5-year after loading follow-up. Eur J Oral Implantol. 2014; 7: 359-369.
- Gonçalves TM, Bortolini S, Martinolli M, Alfenas BF, Peruzzo DC, Natali A, et al. Long-term Short Implants Performance: Systematic Review and Meta-Analysis of the Essential Assessment Parameters. Braz Dent J. 2015; 26: 325-336.
- Nickenig HJ, Eitner S, Rothamel D, Wichmann M, Zöller JE. Possibilities and limitations of implant placement by virtual planning data and surgical guide templates. Int J Comput Dent. 2012; 15: 9-21.
- Schlegel KA, Karascholi T, Fenner M, Nkenke E. [Clinical and radiological results after augmentation procedures - a prospective study]. Mund Kiefer Gesichtschir. 2007; 11: 209-219.
- Kim DH, Rhim R, Li L, Martha J, Swaim BH, Banco RJ, et al. Prospective study of iliac crest bone graft harvest site pain and morbidity. Spine J. 2009; 9: 886-892.
- Nordera P, Spanio di Spilimbergo S, Stenico A, Fornezza U, Volpin L, et al. The cutting-edge technique for safe osteotomies in craniofacial surgery: the piezosurgery bone scalpel. Plast Reconstr Surg. 2007; 120: 1989-1995.
- Vercellotti T. Technological characteristics and clinical indications of piezoelectric bone surgery. Minerva Stomatol. 2004; 53: 207-214.
- Metzger MC, Bormann KH, Schoen R, Gellrich NC, Schmelzeisen R. Inferior alveolar nerve transposition--an in vitro comparison between piezosurgery and conventional bur use. J Oral Implantol. 2006; 32: 19-25.
- Bovi M. Mobilization of the inferior alveolar nerve with simultaneous implant insertion: a new technique. Case report. Int J Periodontics Restorative Dent. 2005; 25: 375-383.
- Luna AH, Passeri LA, de Moraes M, Moreira RW. Endosseous implant placement in conjunction with inferior alveolar nerve transposition: a report of an unusual complication and surgical management. Int J Oral Maxillofac Implants, 2008. 23: 133-136.
- Rosenquist B. Fixture placement posterior to the mental foramen with transpositioning of the inferior alveolar nerve. Int J Oral Maxillofac Implants. 1992; 7: 45-50.
- Kan JY, Lozada JL, Goodacre CJ, Davis WH, Hanisch O. Endosseous implant placement in conjunction with inferior alveolar nerve transposition: an evaluation of neurosensory disturbance. Int J Oral Maxillofac Implants. 1997; 12: 463-471.
- Dellon AL, Mackinnon SE, Crosby PM. Reliability of two-point discrimination measurements. J Hand Surg Am. 1987; 12: 693-696.
- Pria CM, Masood F, Beckerley JM, Carson RE. Study of the inferior alveolar canal and mental foramen on digital panoramic images. J Contemp Dent Pract. 2011; 12: 265-271.
- Kaeppler G, Mast M. Indications for cone-beam computed tomography in the area of oral and maxillofacial surgery. Int J Comput Dent. 2012; 15: 271-286.
