Research Article
Austin J Clin Ophthalmol. 2014;1(6): 1028.
Collateral Vessels after Retinal Vein Occlusion Treated with Intravitreal Bevacizumab
Montero-Moreno JA1,2* and Ruiz-Moreno JM3,4
1Pio Del Rio Hortega University Hospital, Spain
2Retina Unit, Oftalvist Moncloa, Spain
3Department of Ophthalmology, Castilla La Mancha University, Spain
4Baviera Clinic, European Opthalmic Institute, Spain
*Corresponding author: Montero-Moreno JA, Pio Del Rio Hortega University Hospital, Ophthalmology Unit, Calle Dulzaina 2, 47012, Valladolid, Spain
Received: July 28, 2014; Accepted: Aug 04, 2014; Published: Aug 06, 2014
Abstract
Purpose: To report the occurrence of optic disk and retinal collaterals in eyes with macular edema secondary to central (CRVO) and branch retinal vein occlusion (BRVO) treated with intravitreal bevacizumab (IVB).
Material and Methods: Retrospective, interventional study. The files and photographs of 22 eyes from 22 patients with macular edema secondary to BRVO and CRVO treated with IVB were revised.
Results: Fifteen eyes presented BRVO and seven eyes presented CRVO. None of the eyes had been previously treated with laser. Average best-corrected visual acuity improved from 44.8±21 letters to 58.3±22.8 letters by the end of the first year and 56.7±25.5 letters by the end of the second year (p=0.00001 and p=0.005 respectively, Student t test for paired data). The average number of IVB performed during the first year was 4.4±2.5 (range 2 to 13) and 2.1±2.2 (range 1 to 13) during the second year. By the end of the second year, 11 eyes in the BRVO group presented collateral vessels (seven eyes presented optic disk shunts and four eyes presented intraretinal collaterals) and six eyes in the CRVO group presented optic disk shunts.
Conclusion: IVB does not prevent optic nerve and retinal collateralization in eyes treated for macular edema secondary to retinal vein occlusion.
Keywords: Bevacizumab; Collateral Vessels; Optic Disk; Retinal Vein Occlusion; Vascular Endothelial Growth Factor
Introduction
Retinal vein occlusions (RVO) are the most frequent vascular diseases of the retina after diabetic retinopathy [1]. These conditions may frequently cause macular edema and ischemia resulting in reduced visual acuity. During the past 20 years several therapeutic options have been tried such as laser chorioretinal anastomosis, intravitreal and intraluminal recombinant tissue plasminogen activator, isovolemic hemodilution, hyperbaric oxygen therapy and vitrectomy with or without radial optic neurotomy (RON) [2-6]. One of the assumptions of some of these approaches was the creation of veno-venous anastomosis that might provide collateral circulation and thus restore the disturbed venous circulation.
In vivo and in vitro research has shown that vascular endothelial growth factor (VEGF) is over-expressed in eyes with RVO, [7] and that it is significantly correlated with the non-perfused areas and with the severity of macular edema [8]. Anti-VEGF therapy has become a useful tool in the management of macular edema secondary to RVO [9-14], improving visual acuity and reducing severe complications such as neovascular glaucoma. However, early research on eyes treated with intravitreal bevacizumab revealed absence of collateral vessels arising significant concern on the effect of anti VEGF treatment on ischemic retina [15].
We describe a group of laser-naÏve patients with RVO treated with serial intravitreal injections of 1.25mg bevacizumab (IVB) who developed optic disk and intraretinal collaterals during IVB treatment.
Material and Methods
Retrospective, interventional study. The files and fundus photographs of laser-naÏve patients with macular edema secondary to RVO that had been treated with IVB were revised. A complete ocular examination including fluorescein angiography (FA) and Spectral Domain Optical Coherence Tomography (SD-OCT) (Cirrus, Carl Zeiss Meditech, Dublin, CA, USA) was performed at baseline when RVO was diagnosed and IVB treatment was decided. Follow-up evaluations consisted of determination of best-corrected visual acuity (BCVA), intraocular pressure, anterior and posterior segment examination and SD-OCT. Treatment consisted of 1.25mg IVB performed on a “treat and extend” protocol.
Results
Twenty-two patients with macular edema secondary to RVO that had been treated with IVB were identified. Fifteen patients presented with branch retinal vein occlusion [BRVO] (five of them were females) and seven with central retinal vein occlusion [CRVO] (one female). The mean age at baseline was 70±9 years.
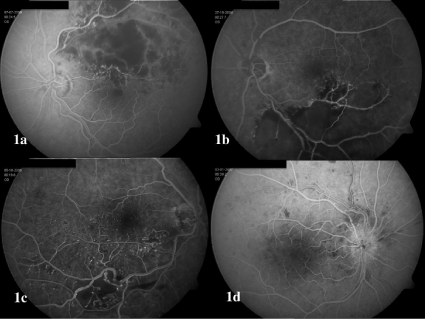
None of the patients had received previous laser treatment. Baseline FA revealed retinal ischemia larger than five optic disk areas in nine eyes with BRVO and in five eyes with CRVO. (Figure 1) One of the eyes with CRVO had been previously unsuccessfully treated by vitrectomy and RON. Basal average BCVA was 44.8±21 Early Treatment Diabetic Retinopathy Study (ETDRS) letters and central macular thickness (CMT) as determined by SD-OCT was 592±242 μm. After 1-year treatment with an average 4.4±2.5 IVB (range 2 to 13), mean BCVA was 58.3±22.8 letters (22 eyes; p=0.00001, Student t test for paired data) and CMT was 313±173 μm (p=0.0004). At 2-years, mean BCVA was 56.7±25.5 ETDRS letters (21 eyes; p=0.005), with 13 treatment-free patients and an average 2.1±2.2 IVB (range 1 to 13). CMT was 300±149 μm (p=0.002). Eight eyes still required anti VEGF therapy during the second year and received an average 7.0±3.6 IVB. By the end of the third year, mean BCVA was 65.2±18.3 ETDRS letters (12 eyes; p=0.0003), with six treatment-free patients and an average 2.3±2.4 IVB (range 1 to 11). CMT was 296±84 μm (p=0.0003).
Figure 1 : Fluorescein angiography in four eyes with retinal vein occlusion prior to treatment with intravitreal bevacizumab. 1a-1b: Branch retinal vein occlusion (BRVO) in two eyes with retinal ischemia larger than five disk areas (DA). 1c: BRVO with retinal ischemia smaller than five DA. 1d: Central retinal vein occlusion (CRVO) with moderate retinal ischemia smaller than five DA.
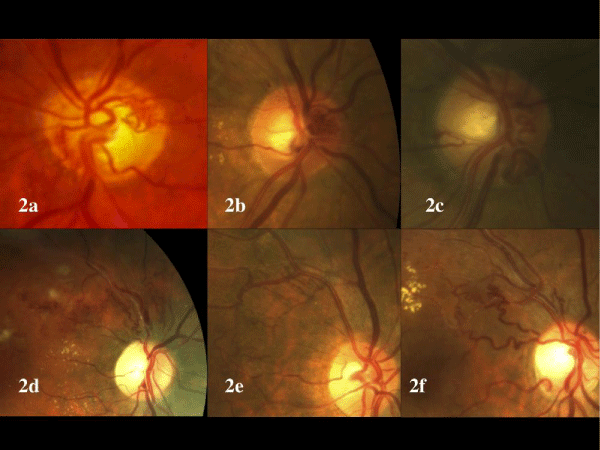
By the end of the second year, 11 eyes in the BRVO group presented collateral vessels (seven presented optic disk shunts and four presented intraretinal collaterals) (Figure 2) and six eyes in the CRVO group presented optic disk shunts (Figure 3). All the eyes with basal retinal ischemia developed collateral vessels. Those eyes that required IVB during the second and third year presented collateral vessels.
Figure 2 : Color photographs from six eyes with branch retinal vein occlusion treated by serial monthly intravitreal bevacizumab (IVB). 2a-2c: TreatmentnaÏve eyes treated by IVB with optic disk collaterals. 2d-2f: Treatment-naÏve eyes treated by IVB with retinal collaterals.
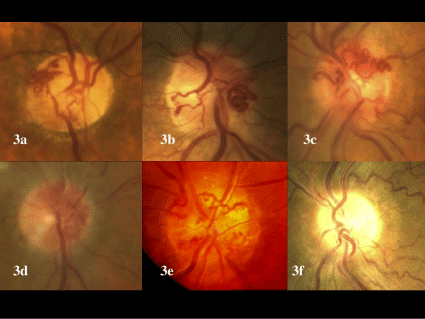
Figure 3 : Color photographs documenting the occurrence of optic disk shunts in eyes with central retinal vein occlusion treated with intravitreal bevacizumab (IVB). 3a-3d: Treatment-naÏve eyes treated by IVB with optic disk collaterals. 3e: This eye had been previously treated by vitrectomy and radial optic neurotomy followed by monthly IVB that did not prevent the occurrence of optic disk shunts. 3f: This eye required IVB during six consecutive months. Optic disk collaterals were not observed.
Discussion
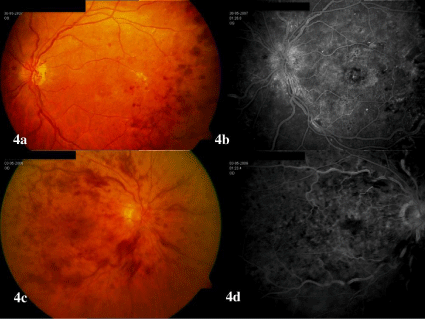
Restoration of venous flow in eyes with RVO is considered to occur by either re-canalization of the obstructed vein or the development of collateral vessels [16]. In fact, the benefits of certain therapeutic procedures such as RON [17] and laser-induced chorioretinal anastomosis [18] were attributed to the formation of collaterals and the amount of new vessels was correlated to the reduction of macular edema [19]. Optic disk collaterals have been described in 77% of the cases with untreated CRVO [20] (Figures 4-5).
Figure 4 : Fundus photograph and fluorescein angiography from two untreated eyes with central retinal vein occlusion (CRVO). 4a-4b: CRVO with collateral optic disk vessels. 4c-4d: CRVO without collateral vessels. Notice the presence of retinal ischemia and macular edema in both eyes (4b and 4d).
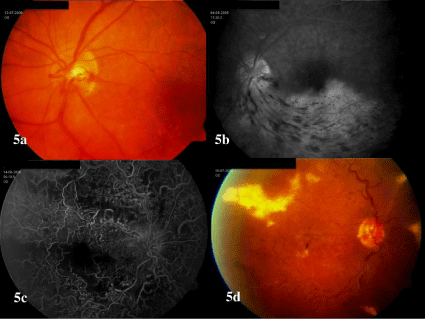
Figure 5 : Fundus photograph and fluorescein angiography from two anti-VEGF-naÏve eyes with branch retinal vein occlusion (5a-5b) and central retinal vein occlusion (5c-5d). Notice the presence of optic disk collaterals in both eyes. 5c-5d: This eye had been treated with radial optic neurotomy.
During the past decade, growing evidence has supported the efficacy and safety of intravitreal anti-VEGF therapy in eyes with macular edema secondary to retinal vascular disease, as suggested by good visual outcomes and limited local and systemic side effects [9- 14]. However, the fear of increasing retinal ischemia by the inhibition of collateral vessels has limited this treatment. Ferrara et al. were unable to observe collateral vessels forming at the optic nerve head after evaluating the effects of IVB on six eyes with macular edema secondary to CRVO with a mean follow-up of 12 months (ranging from 7 to 15 months), concluding that the anti VEGF effects of IVB might have inhibited the formation of collaterals, even though visual acuity gain and reduced macular edema were not otherwise compromised [15]. Similar results were reported by Shah et al. on a series of 9 eyes with CRVO treated with one single injection of 2.5mg bevacizumab followed by panretinal and grid laser [21].
The occurrence of collateral vessels in eyes with RVO after IVB treatment has been previously reported [22]. Spaide [23] and Goldberg [24] reported on the occurrence of collateralization after intravitreal ranibizumab in eyes with BRVO and CRVO, respectively. We have observed a high prevalence of collateralization in our series (17/21 eyes). The occurrence of these collaterals is even more remarkable considering the average number of intravitreal injections performed and that all the eyes that required IVB during the second year developed collaterals. One eye that presented with neovascular glaucoma and BCVA hand movements at baseline, improved to 20 ETDRS letters at year 1 and 2; IVB treatment induced disappearance of anterior segment neovascularization but did not preclude formation of optic disk collaterals.
Goldberg attributed the presence of optic disk shunts in her only case to the severity of the occlusion and chronically impaired re-canalization [24]. Intravitreal bevacizumab helps preventing macular damage secondary to macular edema in eyes with RVO and induces regression of anterior segment neovascularization. However, the limited intravitreal half life of serial bevacizumab injections and the high production of VEGF in the ischemic retina may give way to a slow but progressive appearance of vessels in the retinal surface and the optic disk though they will not give way to a fibrovascular proliferation or distant neovascularization. An alternative hypothesis might be related to the modulation of VEGF effects caused by repeated injections of anti VEGF drugs.
According to our findings, serial IVB in eyes with macular edema secondary to RVO prevents macular edema and neovascular glaucoma and permits the development of retinal and optic disk collaterals.
References
- Klein R, Moss SE, Meuer SM, Klein BE. The 15-year cumulative incidence of retinal vein occlusion: the Beaver Dam Eye Study. See comment in PubMed Commons below Arch Ophthalmol. 2008; 126: 513-518.
- Arevalo JF, Garcia RA, Wu L, Rodriguez FJ, Dalma-Weiszhausz J, Quiroz-Mercado H, et al. Radial optic neurotomy for central retinal vein occlusion: results of the Pan-American Collaborative Retina Study Group (PACORES). Retina. 2008; 28: 1044-1052.
- Dodson PM, Galton DJ, Hamilton AM, Blach RK. Retinal vein occlusion and the prevalence of lipoprotein abnormalities. See comment in PubMed Commons below Br J Ophthalmol. 1982; 66: 161-164.
- Höh AE, Schaal KB, Dithmar S. [Central and branch retinal vein occlusion. Current strategies for treatment in Germany, Austria and Switzerland]. See comment in PubMed Commons below Ophthalmologe. 2007; 104: 290-294.
- Park CH, Scott AW, Fekrat S. Effect of oral pentoxifylline on cystoid macular edema associated with central retinal vein occlusion. See comment in PubMed Commons below Retina. 2007; 27: 1020-1025.
- Park DH, Kim IT. Long-term effects of vitrectomy and internal limiting membrane peeling for macular edema secondary to central retinal vein occlusion and hemiretinal vein occlusion. See comment in PubMed Commons below Retina. 2010; 30: 117-124.
- Koss MJ, Pfister M, Rothweiler F, Michaelis M, Cinatl J, Schubert R, et al. Comparison of cytokine levels from undiluted vitreous of untreated patients with retinal vein occlusion. See comment in PubMed Commons below Acta Ophthalmol. 2012; 90: e98-98e103.
- Noma H, Funatsu H, Yamasaki M, Tsukamoto H, Mimura T, Sone T, et al. Aqueous humour levels of cytokines are correlated to vitreous levels and severity of macular oedema in branch retinal vein occlusion. See comment in PubMed Commons below Eye (Lond). 2008; 22: 42-48.
- Brown DM, Campochiaro PA, Bhisitkul RB, Ho AC, Gray S, Saroj N, et al. Sustained benefits from ranibizumab for macular edema following branch retinal vein occlusion: 12-month outcomes of a phase III study. See comment in PubMed Commons below Ophthalmology. 2011; 118: 1594-1602.
- Campochiaro PA, Brown DM, Awh CC, Lee SY, Gray S, Saroj N, et al. Sustained benefits from ranibizumab for macular edema following central retinal vein occlusion: twelve-month outcomes of a phase III study. See comment in PubMed Commons below Ophthalmology. 2011; 118: 2041-2049.
- Heier JS, Campochiaro PA, Yau L, Li Z, Saroj N, Rubio RG, et al. Ranibizumab for macular edema due to retinal vein occlusions: long-term follow-up in the HORIZON trial. See comment in PubMed Commons below Ophthalmology. 2012; 119: 802-809.
- Campochiaro PA, Sophie R, Pearlman J, Brown DM, Boyer DS, Heier JS, et al. Long-term outcomes in patients with retinal vein occlusion treated with ranibizumab: the RETAIN study. See comment in PubMed Commons below Ophthalmology. 2014; 121: 209-219.
- Heier JS, Clark WL, Boyer DS, Brown DM, Vitti R, Berliner AJ, et al. Intravitreal Aflibercept Injection for Macular Edema Due to Central Retinal Vein Occlusion: Two-Year Results from the COPERNICUS Study. See comment in PubMed Commons below Ophthalmology. 2014; 121: 1414-1420.
- Yuan A, Ahmad BU, Xu D, Singh RP, Kaiser PK, Martin DF, et al. Comparison of intravitreal ranibizumab and bevacizumab for the treatment of macular edema secondary to retinal vein occlusion. See comment in PubMed Commons below Int J Ophthalmol. 2014; 7: 86-91.
- Ferrara DC, Koizumi H, Spaide RF. Early bevacizumab treatment of central retinal vein occlusion. See comment in PubMed Commons below Am J Ophthalmol. 2007; 144: 864-871.
- Green WR, Chan CC, Hutchins GM, Terry JM. Central retinal vein occlusion: a prospective histopathologic study of 29 eyes in 28 cases. Retina. 1981; 1: 27-55.
- García-Arumíi J, Boixadera A, Martinez-Castillo V, Castillo R, Dou A, Corcostegui B, et al. Chorioretinal anastomosis after radial optic neurotomy for central retinal vein occlusion. See comment in PubMed Commons below Arch Ophthalmol. 2003; 121: 1385-1391.
- McAllister IL, Gillies ME, Smithies LA, Rochtchina E, Harper CA, Daniell MD, et al. The Central Retinal Vein Bypass Study: a trial of laser-induced chorioretinal venous anastomosis for central retinal vein occlusion. See comment in PubMed Commons below Ophthalmology. 2010; 117: 954-965.
- Spaide RF, Klancnik JM, Jr., Gross NE. Retinal choroidal collateral circulation after radial optic neurotomy correlated with the lessening of macular edema. Retina. 2004; 24: 356-359.
- Takahashi K, Muraoka K, Kishi S, Shimizu K. Formation of retinochoroidal collaterals in central retinal vein occlusion. See comment in PubMed Commons below Am J Ophthalmol. 1998; 126: 91-99.
- Shah NJ, Shah UN. Long-term effect of early intervention with single intravitreal injection of bevacizumab followed by panretinal and macular grid photocoagulation in central retinal vein occlusion (CRVO) with macular edema: a pilot study. See comment in PubMed Commons below Eye (Lond). 2011; 25: 239-244.
- Wu L, Arevalo JF, Roca JA, Maia M, Berrocal MH, Rodriguez FJ, et al. Comparison of two doses of intravitreal bevacizumab (Avastin) for treatment of macular edema secondary to branch retinal vein occlusion: results from the Pan-American Collaborative Retina Study Group at 6 months of follow-up. Retina. 2008; 28: 212-219.
- Spaide RF, Chang LK, Klancnik JM, Yannuzzi LA, Sorenson J, Slakter JS, et al. Prospective study of intravitreal ranibizumab as a treatment for decreased visual acuity secondary to central retinal vein occlusion. See comment in PubMed Commons below Am J Ophthalmol. 2009; 147: 298-306.
- Goldberg N, Freund KB. Progressive optic nerve collateralization after serial intravitreal ranibizumab injections for central retinal vein occlusion. See comment in PubMed Commons below Retina. 2013; 33: 449-450.