Case Report
Ann Surg Perioper Care. 2016; 1(1): 1004.
Percutaneous Embolization of Thoracic Duct Injury after Esophagectomy
Navarrete A1,2,3*, Espinoza S¹, Jimenez-Toscano M¹, Momblan D¹, Delgado S¹, Ibarzabal A¹ and Lacy AM¹
¹Department of Gastrointestinal Surgery, Hospital Clinic, Barcelona, Spain
²Department of Digestive Surgery, Hospital Militar, Santiago, Chile
³Surgery Department, Faculty of Medicine Clínica Alemana Universidad del Desarrollo, Santiago, Chile
*Corresponding author: Andrés Navarrete Molina, Surgery Department, Faculty of Medicine Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Received: August 28, 2016; Accepted: September 26, 2016; Published: September 28, 2016
Abstract
The development of a chylothorax after an esophagectomy, which occurs after iatrogenic injury of the thoracic duct, is a relatively rare but potentially lethal complication. The management of this type of complication is mainly with conservative management and if no optimal response, surgery is indicate. Surgery has high rates of morbidity band also mortality, that is why minimally invasive management, percutaneous embolization, seems to be an interesting alternative. We present a case of thoracic duct leak after minimally invasive esophagectomy. The leak was firstly managed with conservative approach with partial response, so we decided to do a percutaneous embolization with an optimal outcome.
Keywords: Esophagectomy; Thoracic duct; Leak; Percutaneous Embolization
Introduction
The development of a chylothorax after an esophagectomy is a relatively rare but potentially lethal complication. The incidence of ductal injury during esophageal surgery range from 0% to about 8% [1,2]. The anatomical relation of the thoracic duct and the esophagus plus the numerous anatomic variations, may explain injury during dissection of the posterior mediastinum. Chylothorax has local, immunological and nutritional consequences. Mortality of this complication can be as high as 30% to 50% among patients with untreated chronic chylothorax [3]. That is why optimal management of chylothorax is fundamental for decreasing postoperative mortality.
The management can be divided in three alternatives: conservative, surgical and radiological. Conservative treatment must be initiate at diagnosis and it is based on chest drainage, fasting with total parenteral nutrition with or without the use of analogues of somatostatin. This treatment results in resolution of the chylothorax in 36-61% of cases [4,5]. In cases of high flow output chylothorax or failure of conservative treatment, reoperation is indicated as the next step. Early surgical intervention is avoided by many surgeons, given the high mortality [5]. That is why a minimally invasive approach like percutaneous embolization, is an interesting alternative to surgery with optimal results and lower rates of complications [3]. The first report describing percutaneous treatment of chyle leak with catheterization of the cisterna chyle in humans was published by Cope in 1998 [6]. The technical procedure starts with a radiologic demonstration of the cisterna chyli via pedal lymphography, followed by percutaneous, transperitoneal access to the cisterna using a modified Seldinger technique. The technique consists in inserting the catheter in the cisterna, and then the thoracic duct is opacify with nonionic contrast medium. After identification of the leak, embolization of the duct is perform with micro coils, glues, or both. This has prompted some investigators to believe that percutaneous ablation should be attempted before open mediastinal ligation, reserving the latter for percutaneous failures only [7].
We present a case of chylotorax post-esophagectomy of difficult management that was finally resolved by embolization of the thoracic duct by interventional radiology with optimal results.
Case Presentation
We present a 64 year-old male, with history of tobacco consumption of 50 pack-years. The symptoms of presentation were logic dysphagia. The study started with an upper endoscopy identifying an intraluminal, ulcerated lesion, with a neoproliferative aspect from 25 cm to 33 cm from the dental arch in the esophagus. The biopsy confirmed an adenocarcinoma. The computed tomography (CT) scan showed an endoluminal esophageal mass in the middle third of 9 x 3 cm. The study was completed with a EUS that classified the lesion as a T2N2. With all the studies we decided to initiate neoadjuvant treatment with chemo radiotherapy for five weeks. After finishing treatment, an upper endoscopy was done. It showed an extensive ulcer with significant down staging of the esophageal lesion. A new CT scan was made showing a disappearance of the endoluminal lesion with a slight thickening of the esophageal wall at that level. A minimally invasive total esophagectomy was performed without intraoperative complications. The postoperative biopsy showed a T1bN0 adenocarcinoma. In the postoperative evolution the thoracic drainage had a high output with milky aspect. With the suspicion of a chylothorax we started conservative treatment with total parenteral nutrition and antibiotics with no optimal response. An exploratory thoracoscopy, with clipping of the thoracic duct and talc pleurodesis, was performed. After the procedure, the patient persisted with high drainage output, therefore a lymphography with embolization with lipiodol was indicated (Figure 1A-1D). Thanks to this approach, there was a significant decrease in the drainage output associated with a general improvement of the patient, with pleural drain removal after 5 days (Figure 2).
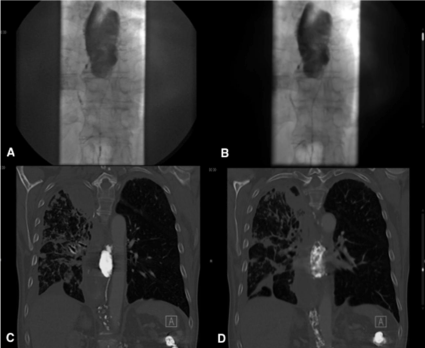
Figure 1: A,B: Identification of thoracic duct leak by contrast injection
previous embolization. C,D: Injection of lipiodol achieving complete occlusion
of the leak.
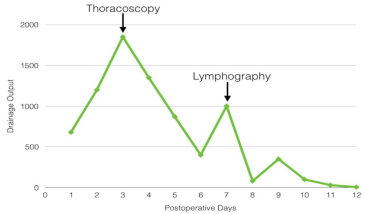
Figure 2: Evolution of the drainage output initially with early thoracoscopy for
management of the leak with only partial response. Therefore lymphography
was the solution, showing optimal outcome.
Discussion
Postoperative chylothorax is a rare but serious complication of esophageal surgical procedures. The rapid loss of chyle is associated with hypovolemia and respiratory problems. If it is not resolve promptly, it can led to malnutrition and immune depression [8]. No single method has proved 100% efficacy and mortality of not treated chylothorax are as high as 50%. Currently, chylothorax remains a challenging problem. The conservative management has an effectiveness of only 50% of cases. In the last decade, pharmacologic adjuvant to conservative therapy has improved the results. Octreotide has showed promise outcomes but not universal success [9]. The classic alternative to conservative manage is surgical ligation of the thoracic duct. Thoracic duct ligation is most commonly performed via thoracotomy, but use of a transabdominal and thorascopic approach has been described. However, high morbidity rates (38%) and mortality (2–16%) have been reported with surgical ligation of the thoracic duct. Furthermore, surgical ligation of the thoracic duct may be ineffective in about 10% of cases [10].
Currently available alternatives to open ligation of the thoracic duct include percutaneous embolization of coils, gelfoam, ethanol and povidone iodine injected directly into the injured thoracic duct. A great advantage over the surgical approach is that surgery may be unable to identify leaks from the main or anomalous accessory duct in comparison to the embolization treatment, where the thoracic duct is identified previous to embolization. The percutaneous approach is a less invasive procedure than surgery and has a success rate of nearly 80%. The complications of lymphangiography are pulmonary oil embolism, hypersensitivity, and lymphatic obstruction, but these are rare and usually minor [8]. In our patient we did not have any secondary effects. Another problem with this approach is the need of lymphangiography to opacify a target for catheterization. The isolation and cannulation of pedal lymphatic vessels require a degree of expertise that may not be available in all contemporary radiology departments. It seems that the low morbidity of percutaneous treatment of chylotorax makes it a reasonable treatment option even before medical management. Embolization of the thoracic duct may even be considering a viable option for patients with persistent chylothorax after fail surgical thoracic duct ligation or even as a first approach alternative [10].
In our case the initial management was total parenteral nutrition plus antibiotics as describe in literature. Although it has a 50% of success, in this case it was not enough to control the high thoracic drainage output. The interventional radiology procedure was successful in identifying the leak. The embolization was done without any posterior complication and the evolution was optimal with decrease of the pleural drainage output. The conclusion that we can learn is that percutaneous embolization is a viable option with low complication rates and excellent results.
References
- Bolger C, Walsh TN, Tanner WA, Keeling P, Hennessy TP. Chylothorax after oesophagectomy. Br J Surg. 1991; 78: 587–588.
- Shah RD, Luketich JD, Schuchert MJ, Christie NA, Pennathur A, Landreneau RJ, et al. Postesophagectomy Chylothorax: Incidence, Risk Factors, and Outcomes. Ann Thorac Surg. 2012; 93: 897–903.
- Chalret du Rieu M, Baulieux J, Rode A, Mabrut JY. Management of postoperative chylothorax. J Visc Surg 2011; 148: 346-352.
- Dugue L, Sauvanet A, Farges O, Goharin A, Le Mee J, Belghiti J. Output of chyle as an indicator of treatment or chylothorax complicating oesophagectomy. Br J Surg. 1998; 85: 1147–1149.
- Merigliano S, Molena D, Ruol A, Zaninotto G, Cagol M, Scappin S, et al. Chylothorax complicating esophagectomy or cancer: a plea for early thoracic duct ligation. J Thorac Cardiovasc Surg. 2000; 119: 453–457.
- Cope C, Salem R, Kaiser LR. Management of chylothorax by percutaneous catheterization and embolization of the thoracic duct: prospective trial. J Vasc Interv Radiol. 1999; 10: 1248-1254.
- Marcon F, Irani K, Aquino T, Saunders JK, Gouge TH, Melis M. Percutaneous treatment of thoracic duct injuries. Surg Endosc. 2011; 25: 2844-2848.
- Lee KH, Jung JS, Cho SB, Lee SH, Kim HJ, Son HS. Duct Embolization with Lipiodol for Chylothorax due to Thoracic Endovascular Aortic Repair with Debranching Procedure. Korean J Thorac Cardiovasc Surg. 2015; 48: 74-77.
- Marthaller KJ, Johnson SP, Pride RM, Ratzer ER, Hollis HW Jr. Percutaneous embolization of thoracic duct injury post-esophagectomy should be considered initial treatment for chylothorax before proceeding with open reexploration. Am J Surg. 2015; 209: 235-239.
- Nadolski GJ, Itkin M. Feasibility of Ultrasound-guided Intranodal Lymphangiogram for Thoracic Duct Embolization. J Vasc Interv Radiol. 2012; 23: 613-616.