Case Report
Austin J Anesthesia and Aalgesia. 2014;2(6): 1034.
Exparel with a Peripheral Nerve Block
Jean Daniel Eloy*, Heidi Boules, James Doran, Kathleen Beebe, Anthony Sifonios and Vanny Le
Department of Anesthesiology, Rutgers/New Jersey Medical School, USA
*Corresponding author: Daniel Eloy, Department of Anesthesiology, Rutgers/New Jersey Medical School, 185 South Orenge Ave, MSB E538, Newark, NJ 07103, USA
Received: July 15, 2014; Accepted: August 15, 2014; Published: August 18, 2014
Abstract
Acute postoperative pain is primarily managed with opioids. In this case, we present the successful postoperative pain management of a patient post left upper extremity sarcoma resection with the use of Exparel via an Infra clavicular nerve block. This case also highlights an alternative to continuous peripheral nerve blocks with their associated risks and complications and illustrates a multimodal approach to acute postoperative pain management in which non-opioid adjuvants are used to achieve an opioid sparing and even opioid free regiment. The case also suggests that an opioid free approach in the treatment of post surgical pain is feasible and should be considered especially when incorporating regional anesthesia as part of a multimodal approach.
Case Presentation
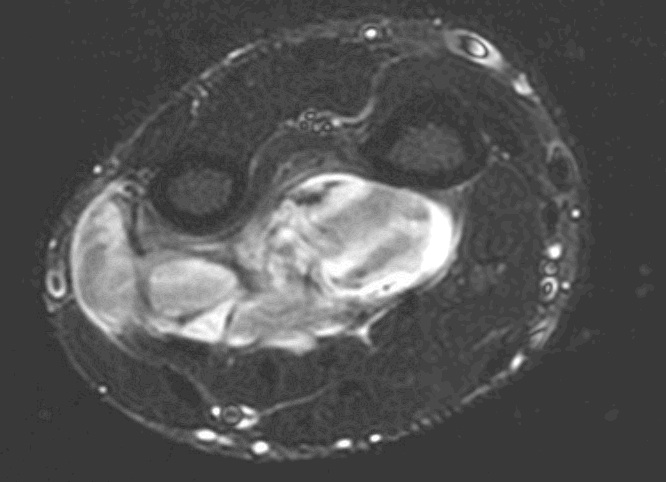
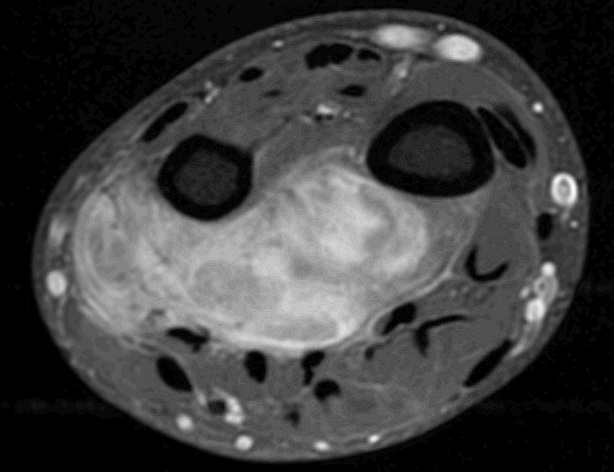
A 27-year-old 78 kg male presented for a radical resection of a left forearm sarcoma. The patient completed chemotherapy for the sarcoma three months prior to the scheduled surgery without complications. His medical history was pertinent for bipolar disorder and depression and a past history of alcohol and illicit substance abuse, which he had been rehabilitated for four years prior to surgery. The patient's surgical history was limited to mediport insertion and left forearm biopsy, which were performed under general anesthesia without complications. MRI of his left upper extremity revealed a 7 cm x 5.6 cm x 3.5cmmulti-loculated, necrotic tumor originating 4 mm proximal to the radial carpal joint. The mass was lying on the cortex of both the radial and ulnar shafts along the interosseous membrane. The lesion was noted to be deep to the flexor digitorum profundus, the flexor carpi ulnaris and the flexor pollicus longus. The median, ulna, and radial nerves along with the radial artery were not encased by tumor but adjacent to the mass (See MRI 1&2).
The patient met with the anesthesia care team prior to surgery in order to explore non-opioid options in the perioperative period. Given the patient's social history, he had expressed to the surgical and anesthetic teams his desire to undergo this procedure and the period of recovery without the use of opioids, except when absolutely necessary. Our plan was to perform a preoperative left brachial plexus block with a catheter using ultrasound guidance to provide both intra operative as well as postoperative analgesia.
On the day of surgery, the patient was brought to the operating room, placed on standard monitors and given supplemental oxygen in preparation for the nerve block. He was sedated with 2 mg midazolam intravenously. An infra clavicular Nerve block was performed with successful blockade of the brachial plexus [1]. A total of 20 ml of 1.3 % Exparel®, 266 mg, was delivered to the site in a single dose. Additionally, a perineural catheter was inserted; however, no additional local anesthetic was injected via this catheter. The catheter was placed to provide a route for rescue medication to be injected, should he require additional local anesthetic.
General anesthesia was induced and the sarcoma was subsequently resected uneventfully. The use of opioid was limited to 100 mcg of fentanyl for the purpose of tracheal intubation. The patient also received 30 mg of Ketorolac and a continuous Ketamine infusion of 20 mg/hr for the duration of the case [2]. Anesthesia was maintained with a 50% mixture O2/Air and Isofluorane. The patient was extubated without complications and received no additional opioids during the immediate postoperative period.
The patient was admitted to a surgical floor to complete his recovery where he was followed by the acute pain management service. He was placed prophylactically on acetaminophen 1000 mg PO Q8 hours, ketorolac 30mg IV Q6 hours and gabapentin 300mg PO Q8 hours. For the first 24 hours after surgery, he reported a score of zero out of ten pain score on the Visual Analog Scale (VAS). He reported an inability to flex or extend his fingers, which reflected a degree of motor blockade. This motor blockade completely resolved over 24 hours. At 48 hours post-op, the patient reported a maximum score of two out of ten VAS pain scoreand no residualmotor blockade. Finally, by 72 hours post-op, the patient reported a maximum score of five out of ten VAS pain score and stated that there was no residual numbness in the blocked arm. The indwelling infra clavicular catheter was removed and the patient was discharged home. Within the immediate 72 hours post-op, the patient did not require any opioid supplementation nor was the infra clavicular catheter bol used with additional local anesthetic.
Figure 1
Figure 2
Discussion
Exparel® (liposome bupivacaine, extended release, Pacira Pharmaceuticals, Parsippany, NJ)) is an injectable suspension of bupivacaine that exists in a honeycomb like structure of microscopic spherical, mulitivesicular liposome's (Depo Foam® drug delivery system). Bupivacaine is released from the DepoFoam particles by a complex mechanism that involves the reorganization of the barrier lipid membranes [3]. It was designed to provide prolonged pain relief via single dose administration. Exparel® is not FDA approved at this time for regional anesthesia. An IND exemption was granted after request made to the FDA.
Gorfine et al. studied Exparel® in 186 patients undergoing hemorrhoidectomy during a multicenter, randomized, double blind, placebo control study and found statistically significant reduction in pain scores over 72 hours. The authors reported greater patient satisfaction, less opioid use postoperatively and a longer median time to first opioid use in the Exparel® group [4].
High plasma concentrations of local anesthetics and cardiac toxicity are a concern, especially when using bupivacaine. Bergese et al. studied the cardiovascular effects in adult (ASA 1-3) patients undergoing unilateral TKA under general anesthesia. Bupivacaine doses of 150, 300, 450, and 600 mgs were studied and ECGs were performed at baseline and repeated at 4 hour (initial) and 12 hour intervals out to 96 hours post dose. No clinically relevant ECG changes or cardiac events were noted [5].
This case demonstrates a multimodal approach in the management of postoperative pain [6]. Although the goal of multimodal analgesia is the reduction in opiate use preoperatively; this case suggests that an opioid free regimen is feasible. The administration of intra operative sub-anesthetic dose of ketamine has been proven to reduce opioid consumption and pain scores in the postoperative setting [7]. Continuation of a low dose ketamine infusion in the postoperative setting has also been shown to decrease opioid use limiting adverse effects associated with opioid administration [8]. Richman et al. showed that continuous peripheral nerve blocks provide superior pain control to opioids, but the use peripheral nerve blocks, continuous or otherwise single injections in postoperative pain management is paramount [9].
This case report seems to indicate that a single dose of Liposomal Bupivacaine of 266 mg injected as part of an infra clavicular nerve block provides adequate analgesia for 3 days postoperatively. Pain caused by inflammatory mediators was treated with Acetaminophen 1000 mg every 8 hours for 2 days. A standing dose of Ketorolac 30 mg every 8 hours was added as part of this opioid sparing strategy as well. Gabapentin is a structural analog of Gaba-aminobutyric acid that binds to the alpha-2 delta subunit of voltage- gated calcium channels used in the treatment of chronic neuropathic pain. However, there is evidence to suggest that it reduces pain in the acute postoperative period [10-12]. In this case, a standard dose of 300 mg every 8 hours was used as part of a multimodal analgesic technique. Because one of the side effects of gabapentin is increased sedation and sleepiness, its use in older patients may require judicious dosage.
In conclusion, the use of Liposomal Bupivacaine (Exparel®) seems to provide safe and effective analgesia when used in a single perineural injection. Since the duration of analgesia provided by a single injection was approximately 72 hours, continuous peripheral techniques may not always be warranted. Exparel® has been FDA approved since 2011 with the indication for injection into the surgical site for the purpose of postoperative analgesia [13-15]. However, Exparel® has not yet been approved for regional anesthesia. This case gives evidence that Exparel® may be used successfully for regional anesthesia in a single injection. This case also provides a model for treating postoperative acute pain in a multimodal approach incorporating regional anesthesia without the known side effects of opioids and risks associated with continuous peripheral nerve blocks.
References
- Sandhu NS, Maharlouei B, Patel B, Erkulwater E, Medabalmi P. Simultaneous Bilateral Infraclavicular Brachial Plexus Blocks with Low-dose Lidocaine Using Ultrasound Guidance. Anesthesiology. 2006; 104: 199-201.
- Subramaniam K, Subramaniam B, Steinbrook RA. Ketamine as adjuvant analgesic to opioids: a quantitative and qualitative systematic review. Anesth Analg. 2004; 99: 482-495, table of contents.
- Davidson EM, Barenholz Y, Cohen R, Haroutiunian S, Kagan L, Ginosar Y. High-dose bupivacaine remotely loaded into multivesicular liposomes demonstrates slow drug release without systemic toxic plasma concentrations after subcutaneous administration in humans. Anesth Analg. 2010; 110: 1018-1023.
- Gorfine SR, Onel E, Patou G, Krivokapic ZV. Bupivacaine extended-release liposome injection for prolonged postsurgical analgesia in patients undergoing hemorrhoidectomy: a multicenter, randomized, double blind, and placebo-controlled trial. Dis Colon Rectum. 2011; 54: 1552-1559.
- Bergese SD, Onel E, Morren M, Morganroth J. Bupivacaine extended-release liposome injection exhibits a favorable cardiac safety profile. Reg Anesth Pain Med. 2012; 37: 145-151.
- Chelly JE, Ploskanych T, Dai F, Nelson JB. Multimodal analgesic approach incorporating paravertebral Bloks for open radical retropubic prostatectomy: a randomized double-blinded placebo-controlled study. Can J Anesth. 2011; 58: 371-378.
- Webb AR, Skinner BS, Leong S, Kolawole H, Crofts T, Taverner M, et al. The Addition of small-dose ketamine infusion to Tramadol for postoperative analgesia: A Double-Blinded, Placebo-Controlled, Randomized Trial After Abdominal Surgery. Anesth and Analg. 2007; 104:912-917.
- Bell RF, Dahl JB, Moore RA, Kalso E. Peri-operative ketamine for acute post-operative pain: a quantitative and qualitative systematic review (Cochrane review). Acta Anaesthesiol Scand. 2005; 49: 1405-1428.
- Richman JM, Liu SS, Courpas G, Wong R, Rowlingson AJ, McGready J, et al. Does continuous peripheral nerve block provide superior pain control to opioids? A meta-analysis. Anesth Analg. 2006; 102: 248-257.
- Turan A, Karamanlioglu B, Memis D, Hamamcioglu MK, Tükenmez B, Pamukçu Z, et al. Analgesic effects of gabapentin after spinal surgery. Anesthesiology. 2004; 100: 935-938.
- Zakine J, Samarcq D, Lorne E, Moubarak M, Montravers P, Beloucif S, et al. Postoperative Ketamine Administration Decreases Morphine Consumption in Major Abdominal Surgery: A Prospective, Randomized, Double-Blinded, Controlled Study. Anesth Analg. 2008; 106: 1856-1861.
- Chahar P, Cummings KC. Liposomal bupivacaine: a review of a new bupivacaine formulation. J Pain Res. 2012; 5: 257-264.
- Sen H, Sizlan A, Yanarates O, Emirkadi H, Ozkan S, Dagli G, et al. A comparison of gabapentin and ketamine in acute and chronic pain after hysterectomy. Anesth Analg. 2009; 109: 1645-1650.
- Richard BM, Rickert DE, Doolittle D, Mize A, Liu J, Lawson CF. Pharmacokinetic Compatibility Study of Lidocaine with EXPAREL in Yucatan Miniature Pigs. ISRN Pharm. 2011; 2011: 582351.
- Cohen SM. Extended Pain Relief Trial Utilizing infiltration of EXPAREL, a long-acting multivesicular liposome formulation of bupivacaine: a Phase IV health economic trial in adult patients undergoing open colectomy. Journal of pain Research. 2012; 5: 567-572.