Research Article
Austin J Anesthesia and Analgesia. 2014;2(3): 1020.
Retrospective Pharmacoeconomic Analysis of Perioperative use of Intraveneous Acetaminophen
Anita Gupta1*, Lisa K Lee1, Sonali Rao1, Snigdha Aancha1, Cyrus Dadachanji1, Kirtanaa Voralu2
1Division of Pain Medicine & Regional Anesthesiology, Department of Anesthesiology and Perioperative Medicine, Drexel University College of Medicine, USA
2Clinical Research Group, Drexel University College of Medicine, USA
*Corresponding author: Anita Gupta, Pain Medicine and Regional Anesthesiology, Drexel University College of Medicine/ Hahnemann University Hospital, 230 N. Broad St Mailstop 310, Philadelphia PA 19102.
Received: February 18, 2014; Accepted: March 31, 2014; Published: April 10, 2014
Abstract
Background: Pain is a growing public health problem that costs society $560–$635 billion annually. Using a potent analgesic to alleviate the postoperative pain may result in substantial analgesia and enhanced patient satisfaction. The benefits are often challenging to decipher in terms of cost reduction and necessity to improve quality of care. Furthermore, commonly used mediations like non–steroidal anti–inflammatory drugs (NSAIDs) and opioids are associated with potentially adverse side effects. The recent release of intravenous (IV) acetaminophen in the United States has raised concerns related to its analgesic efficiency and cost–effectiveness. The aim of this retrospective chart review is to study the perioperative use of IV acetaminophen and its potential for cost effectiveness when used in this setting.
Methods: We performed a retrospective cohort study of all patients who had undergone surgeries at Drexel University College of Medicine⁄Hahnemann University hospital from September 2011 to February 2012. This review evaluated cost of IV acetaminophen per patient, cost of other analgesics (NSAIDs, Opioids) and total cost of analgesics used per patient. In addition, we evaluated visual analog scores (VAS), length of hospital stay, global patient satisfaction, and opioid related side–effect. The groups were compared with Chisquared test and p–values were reported.
Results: Analysis of the retrospective data showed that the majority of the study population had were ASA grade II (51%) and 74% of the patients received acetaminophen as an preoperative analgesic. All patients, 80 (100%) received intraoperative analgesics which included a combination of drugs such as fentanyl, morphine and hydromorphone. In addition, postoperatively, 36 (45%) did not receive analgesia and 19 (24%) had regional anesthetic nerve blocks. Seventy one (88%) of patients did not have any adverse events; post–operative nausea was noticed in 5 (6.25%) patients and vomiting in 1 (1.25%) of patients.
Conclusion: This retrospective pharmacoeconomic review suggests that the IV formulation of acetaminophen increased the total cost of analgesics used perioperatively. Although, it may be cost effective since there is a less total opioid consumption and subsequently fewer opioid related side effects and potentially decreased length of stay. Further complete randomized controlled studies are needed to delineate the role and cost effectiveness of multimodal analgesia with the use of IV acetaminophen.
Keywords: Cost; Acetaminophen; Efficacy; Outcomes; Surgery; Postoperative
Introduction
Intravenous acetaminophen is an analgesic and antipyretic agent that has been recommended worldwide as a first–line agent for the control of pain and fever in adults and children. While oral and rectal acetaminophen has been on the market for many decades, IV acetaminophen was introduced only about 10 years ago in Europe and 2 years ago in the United States. The key advantage of IV acetaminophen is that approximeately 1 gram is associated with about twice the plasma and effective site concentrations compared to 1 gram of its oral or rectal formulations. The higher concentrations lead to greater central nervous system penetration which is consistent with the superior analgesic efficacy seen with IV compared with oral acetaminophen in the surgical setting [1]. Pharmacoeconomic data are particularly useful for new drug reviews, where branded pharmaceuticals were mostly responsible for the 200% increase in prescription drug costs from 1990 through 2000 [2]. Analgesia is one potential challenge—use of a potent analgesic to reduce postoperative pain may result in significant analgesia and improved patient satisfaction, but it is difficult to translate these effects in figures of cost reduction or improvements in efficiency. In fact, the opposite may be true because the most common classes of analgesics used in the hospital— specifically, nonsteroidal anti–inflammatory drugs (NSAIDs) and opioids—are associated with significant adverse drug reactions which could pose a significant additional economic burden. Since 2005, various studies have been carried out to know the effectiveness of potentially costly adverse drug events (ADEs) [2] of intravenous acetaminophen. These studies clearly establish the analgesic efficacy of intravenous acetaminophen as well as the safety profile of this drug, and also help to decrease the requirements of other analgesics for pain control [3,4]. In double–blind clinical trials, single or multiple doses of intravenous acetaminophen, 1 gram generally provided significantly better analgesic efficacy than placebo treatment in adult patients who had undergone dental, orthopedic or gynecological surgeries [5–8]. Furthermore, where evaluated, intravenous acetaminophen 1 gram generally reduced need for opioid rescue medication [9]. The intravenous route is especially advantageous in postsurgical situations when oral (e.g. infections with severe fever or vomiting) or rectal (e.g. high variability in uptake and bioavailability) routes are not suitable or effective [6]. IV acetaminophen is a costly drug and 1gram vial costs $10 as compared to 1 gram oral that costs $0.80. Though the efficacy and safety of this drug has been established by the recent studies, none of the studies have tried to know the cost effectiveness of this drug.
In our study, we performed a retrospective chart review and pharmcoeconomic analysis of patients that were given perioperative IV acetaminophen. The recent release of IV acetaminophen in the United States has anesthesiologists, surgeons, and facilities questioning the analgesic and cost–effectiveness of intravenous acetaminophen perioperative use in regard to pain relief, opioid utilization, and Post Anesthesia Care Unit (PACU) discharge times. The objective of this study is to determine the cost effectiveness of perioperative use of IV acetaminophen in various surgical procedures compared to other analgesics such as NSAIDs and opioids.
Methods
We conducted a retrospective cohort study evaluating costs of IV acetaminophen per patient, cost of other analgesics (Opioids, NSAIDs, etc.) per patient, and total cost of analgesics used per patient. In addition, we reviewed, visual analog scores (pre and postoperative), length of hospital stay, global patient satisfaction, opioid related side–effects (e.g. nausea, vomiting, changes in blood pressure, delirium). The Drexel University Institutional Review Board approval was obtained prior to patient selection. Patients who had surgery and received IV acetaminophen between September 2011 to February 2012 were selected from the operating room (OR) pharmacy list and schedule. Furthermore, patient's medical history, type of surgery, duration of surgery, hospital stay, medications,substance abuse, ASA status, pre and post–operative pain scores, use of analgesics, complications, name of surgeon, anesthesiologist and CRNA and patient satisfaction, if documented, were collected from the medical record.
Inclusion and exclusion critieria
The following were the inclusion criteria for individuals into the study: 16– 65 years of age, males and females, ASA physical status I, II, or III, undergone surgical procedure, availability of medical charts, documentation of pain scores. The following were the exclusion criteria for individuals into the study: history of substance abuse, history of chronic pain greater than three months, nondocumentation of pain scores, pregnancy, impaired liver function, psychiatric disorder.
Statistical analysis
No sample size or power calculation was performed, all eligible patients who had undergone surgery at Drexel University College of Medicine⁄Hahnemann University Hospital from September 2011 to February 2012 were included in this study. An estimation of 100 medical charts was reviewed and 80 patients met the eligibility criteria. Data analysis was performed with SPSS (IBM Corp. Released 2011. IBM SPSS Statistics for Windows, Version 20.0. Armonk, NY: IBM Corp). Mean, standard deviation (SD), median and range were obtained for age, length of hospital stay, length of PACU stay and VAS. Number of observations and percentages were obtained for type of surgery, ASA status, administration of analgesics and regional blocks, and adverse events. The groups were compared with Chisquared test and p–values were reported.
Results
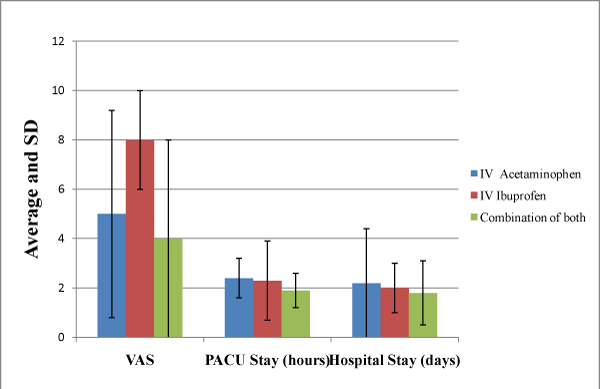
The analysis included data from 80 patients who underwent surgeries at Drexel University College of Medicine⁄Hahnemann University Hospital from September 2011 to February 2012. Results showed that there were 76 (95%) orthopedic surgeries and 4 (5%) plastic surgeries included in the study. The patient demographics and adverse events are presented in Table 1. The mean age was 47 years old (standard deviation 15). The mean postoperative VAS was 5 (standard deviation 4). Length of stay in the PACU and the hospital were similar with a mean of 3 days (standard deviation2). Forty one (51%) of the study population had an ASA of II. Fifty nine (74%) of patients received IV acetaminophen for pain control. Thirty six (45%) of patients did not receive postoperative analgesics; 19(24%) patients had regional blocks. Seventy–one(88%) of patients did not have any adverse events; postoperative nausea occurred in 5 (6.25%) of patients and vomiting occurred in 1(1.25%) of patients. The average pain score was 5, (standard deviation 4) for the acetaminophen group, the mean was 8 (standard deviation 3) for the ibuprofen group and the mean was 4 (standard deviation 5) for combination of both groups (Figure 1 and Table 2). The cost of 1000 mg IV acetaminophen is $12 as opposed to $0.80 for 1000 mg oral acetaminophen. The cost of 800 mg IV Ibuprofen is $11. The cost of PCA Hydromorphone 1mg/ml 30 ml cartridge is $20.49 and PCA Morphine 5 mg⁄ml 30 ml cartridge is $7.90 (Table 3).
Characteristics
n (%)
Mean (SD)
Median (Range)
p-value
Age (years)
80 (100)
47.2 (14.66)
48 (20-83)
-
Length of hospital stay (days)
80 (100)
3 (2)
1 (1-13)
-
Length of PACU stay (hours)
80 (100)
3 (2)
3 (1-7)
-
VAS
80 (100)
5 (4)
5 (0-10)
-
ASA stage
I
12 (15.0)
-
-
<0.001
II
41 (51.25)
III
27 (33.75)
Analgesics (IV)
Acetaminophen
59 (73.75)
-
-
<0.001
Ibuprofen
5 (6.25)
Combination of both
16 (20.0)
Post-Operative Analgesics
None
36 (45.0)
-
-
<0.001
Fentanyl
13 (16.25)
Others
7 (8.75)
Combination of all
24 (30.0)
Regional Blocks
No
61 (76.25)
-
-
<0.001
Yes
19 (23.75)
Adverse events
None
71 (88.75)
-
-
<0.001
Nausea
5 (6.25)
Vomiting
1 (1.25)
Combination of both
3 (3.75)
Table 1: Patient Demographics and Adverse Events.
Figure 1: VAS and Length of Hospital Stay from September 2011 to Februrary 2012.
Pain Scores (VAS)
N
Mean VAS (SD)
95 % Confidence Interval of mean
F-test (df)
p-value
Analgesics (IV)
Acetaminophen
Ibuprofen
Combination of both
59
5
16
5 (4)
8 (3)
4 (5)
3, 5
4, 10
1, 6
1.59 (2, 77)
0.210
Length of PACU stay
N
Mean Hours (SD)
95 % Confidence Interval of mean
F-test (df)
p-value
Analgesics (IV)
Acetaminophen
Ibuprofen
Combination of both
59
5
16
2 (2)
2 (1)
2 (1)
2, 3
1, 3
1, 3
0.20 (2, 77)
0.821
Table 2: Pain scores (VAS) and Length of stay in the PACU Comparison of Intravenous Analgesics (n=80).
Drug
Formulation
Strength
Cost per unit (Dollars)
Daily cost (Dollars)
Fentanyl
Ampule
50 mg/mL
1.63
13.02
Vial
50 mg/mL
0.95
7.6
Hydromorphone
Syringe
1 mg/mL
1.71
13.68
Syringe
2 mg/mL
1.85
7.4
Vial
2 mg/mL
1.01
4.05
Morphine
Syringe
2 mg/mL
1.53
30.6
Syringe
4 mg/mL
1.54
15.4
Vial
5 mg/mL
0.99
7392
Vial
10 mg/mL
1.14
4.56
IV Acetaminophen
Vial
1000 mg in 100 mL
11.4
45.6
IV Ibuprofen
Vial
800 mg
10.5
42
IV Ketorolac
Vial
30 mg/mL
0.81
3023
Vial
60 mg in 2 mL
0.95
3.81
Table 3: Estimated Daily Costs of Analgesics (Data obtained from Drexel University College of dicine/Hahnemann University Hospital, Inpatient Pharmacy. Based Upone Average Wholesale Price (AWP) from Red Book Edition 2012).
Multimodal analgesia is characterized by simultaneous administration of different classes of analgesic medication to target different pathways involved in pain response [10]. Advances in our understanding of the pathophysiology of postoperative pain have led to the development of effective perioperative analgesic regimens. It is now well recognized that pain is a complex and multifactorial phenomenon and therefore requires a multimodal therapy [11]. The concept of multimodal or balanced analgesia suggests thatcombinations of several analgesics of different classes and different sites of analgesic administration rather than single analgesic or single technique provide superior pain relief with reduced analgesic–related side effect [11–13]. In addition to opioids, the analgesic modalities available for multimodal analgesia include regional or local analgesia techniques such as epidural analgesia and peripheral nerve blocks as well as wound infiltration and intra–articular or intra–cavity administration of local anesthetics. In addition, cyclooxygenase (COX) enzyme blockers such as acetaminophen, nonsteroidal antiinflammatory drugs (NSAIDs) or COX–2– specific inhibitors are becoming popular. Recently, there has been an increased interest in using analgesic adjuncts such as N–methyl–D–aspartate (NMDA) receptor antagonists (e.g. ketamine and dextromethorphan), a2 agonists (e.g., clonidine and dexmedetomidine), anticonvulsants (e.g., gabapentin and pregabalin), and corticosteroids. While oral and rectal acetaminophen has been on the market for many decades, IV acetaminophen was introduced only about 10 years ago in Europe and 2 years ago in the United States. The key advantage of IV acetaminophen seems to be that 1 g of IV acetaminophen is associated with about twice the plasma and effect site concentrations as 1 g of its oral or rectal applications, resulting in greater central nervous system penetration [14], which corroborates the superior analgesic efficacy seen with IV compared to oral acetaminophen in the surgical setting [15].
We studied the frequency of different supplemental pain medications among the patients who had been managed with multimodal analgesia for their acute pain in our hospital setting. At Drexel University College of Medicine⁄Hahnemann University Hospital, IV acetaminophen was used significantly more often than IV ibuprofen or combination of these two medications in the perioperative period. Significant number of these patients did not require pain medications during their stay in the recovery room. Our finding with respect to the more number of patients who did not require opioid treatment in Post–Operative Care Unit was similar to the study of [16]. With regard to the expense of current treatments, the cost of each vial of 1000 mg IV acetaminophen is $12 as opposed to $0.80 for 1000 mg oral. However, the use of IV can be more costeffective if it results in shortening of PACU stay by providing better pain relief and/or by decreasing the number of patients who require opioids and subsequently lowering the incidence of opioid induced nausea or vomiting. In addition, staffing costs of PACU for 2 hours is relatively equivalent to the cost of staffing for 24 hours on the regular medical floor [16]. Our analysis may potentially demonstrate that use of multimodal analgesia may significantly reduce the usage of postoperative analgesics and adverse events. Similarly, Memis et al [17] studied the analgesic efficacy of intravenous acetaminophen, its side effects, time taken to extubate and need for postop analgesics when used as an adjuvant (AM group) in comparison with intravenous meperidine (M group) in intensive care units after major surgery. The intravenous meperidine with adjuvant intravenous acetaminophen administration is associated with better postoperative analgesia and earlier time to extubation to that induced by meperidine alone after major surgery operation. In addition, postoperative nausea–vomiting and sedation were significantly lower in group acetaminophen – meperidine when compared with meperidine only. Furthermore, Atef et al [18] concluded intravenous acetaminophen administered regularly in adult patients with moderate to severe pain after tonsillectomy provided rapid and effective analgesia and was well tolerated. This study proves that intravenous acetaminophen given regularly had a substantial analgesic efficacy in the management of pain and opioid sparing effect during the first 24 h after tonsillectomy in adults. This well acknowledged opioid sparing effect is of great importance owing to the wide range of unwanted side effects of opioids––which could be lethal––particularly in the first hours after surgery like respiratory center depression, dizziness, PONV, constipation and voiding difficulties; thus any medication that can replace or reduce the total dose of opioids should be considered while planning the multimodal analgesia regimen. Sinatra et al [4] concluded intravenous acetaminophen administered over a 24 hours period in patients with moderate to severe pain after orthopedic surgery was well tolerated and reduced the consumption of postoperative morphine consumption. Intravenous acetaminophen was consistently superior to placebo for the main efficacy criterion of pain relief, as well as for pain intensity which changes from 15 min to 6 h after the first dose and throughout the 24–h evaluation period after repeated dose administration. Apfel et al [1] conducted a systematic review and Meta –analysis to identify randomized trials of IV acetaminophen versus a placebo control on the effect of nausea and vomiting. They demonstrated that prophylactic IV acetaminophen reduces postoperative nausea and vomiting with an effect size that compares well with data known from other antiemetics. The results suggest that the antiemetic effect of IV acetaminophen is not facilitated through the reduction of postoperative opioid intake, but through direct mechanisms or through the reduction of postsurgical pain. Cakan T, et al [19] conducted a retrospective case control matched cohort study with patients undergoing cardiothoracic surgery with midline sternotomy. Fast–track patients with IV acetaminophen on board had significantly shorter times to extubation and shorter lengths of stay in the post–anesthetic or ICU, intermediate care unit and hospital. Similarly, in 2006, Allashemi [20] showed an earlier readiness for PACU discharge with median time of 15 minutes for IV acetaminophen group versus 25 minutes for the IM meperidine group. In our study, we have been able to demonstrate that within our institution, the current preference of our anesthesia providers is the utilization of multimodal analgesia during the perioperative period. Furthermore, our preliminary pharmcoeconomic analysis may provide an initiative to further evaluate if indeed a cost difference is seen in the long term care of surgical patients. Improving patient satisfaction for surgical patients is of growing importance of improving the quality of care we deliver. Utilizing cost effective methods and improving quality via multimodal analagesia may provide improvement in patient satisfaction overall. Certainly, further randomized controlled studies are necessary to corroborate our preliminary research and to delineate more effectively the role of multimodal analgesia and the cost–effectiveness analysis of these regimens.
Study Finances
No funding was provided for this research. Any related expenses in conducting medical chart review, data collection and analysis was financed internally by the Drexel University Collge of Medicine, Department of Anesthesiology and Perioperative Medicine.
Acknowledgement
Sharon Mindel, PharmD, Director of Pharmacy at Drexel University College of Medicine⁄Hahnemann University Hospital assisted with the cost analysis and average wholesale prices for the medications discussed in the study.
Conflict of Interest
No conflicts of interest exist for this research and any related conflicts were disclosed to the Office of Research at Drexel University
References
- Apfel C C, Turan A, Souza K, Pergolizzi J, Hornuss C. Intravenous acetaminophen reduces postoperative nausea and vomiting: a systematic review and meta-analysis. Pain. 2013; 154: 677-689.
- Jahr JS, Filocamo P, Singh S. Intravenous acetaminophen: a review of pharmacoeconomic science for perioperative use. Am J Ther. 2013; 20: 189- 199.
- Macario A, Royal MA. et al. A literature review of randomized clinical trials of intravenous acetaminophen (paracetamol) for acute postoperative pain. Pain Pract. 2011; 11: 290-296.
- Sinatra RS, Jahr JS, Reynolds LW, Viscusi ER, Groudine SB, Payen- Champenois C. Eficacy and safety of single and repeated administration of 1 gram intravenous acetaminophen injection (paracetamol) for pain management after major orthopedic surgery. Anesthesiology. 2005; 102: 822-831.
- Duggan ST, Scott LJ. Intravenous paracetamol (acetaminophen). Drugs. 2009; 69: 101-113.
- Moon YE, Lee YK, Lee J, Moon DE. The effects of preoperative intravenous acetaminophen in patients undergoing abdominal hysterectomy. Arch Gynecol Obstet. 2011; 284: 1455-1460.
- McNicol ED, Tzortzopoulou A, Cepeda MS, Francia MB, Farhat T, Schumann R. Single-dose intravenous paracetamol or propacetamol for prevention or treatment of postoperative pain: a systematic review and meta-analysis. Br J Anaesth. 2011; 106: 764-775.
- Sinatra RS, Jahr JS, Reynolds L, Groudine SB, Royal MA, Breitmeyer JB, et al., Intravenous acetaminophen for pain after major orthopedic surgery: an expanded analysis. Pain Pract. 2012; 12: 357-365.
- Van Aken H, Thys L, Veekman L, Buerkle H. Assessing analgesia in single and repeated administrations of propacetamol for postoperative pain: comparison with morphine after dental surgery. AnesthAnalg, 2004; 98: 159- 165.
- Zafar N, Davies R, Greenslade GL, Dixon AR.The evolution of analgesia in an 'accelerated' recovery programme for resectional laparoscopic colorectal surgery with anastomosis. Colorectal Dis. 2010; 12: 119-124.
- Woolf C.J. Pain: moving from symptom control toward mechanism-speciic pharmacologic management. Ann Intern Med. 2004; 140: 441-451.
- Kehlet H, Dahl JB.The value of "multimodal" or "balanced analgesia" in postoperative pain treatment. AnesthAnalg. 1993; 77: 1048-1056.
- Kehlet H, M. Werner, and F. Perkins, Balanced analgesia: what is it and what are its advantages in postoperative pain?. Drugs. 1999; 58: 793-797.
- Singla NK1, Parulan C, Samson R, Hutchinson J, Bushnell R, Beja EG, et al. Plasma and cerebrospinal luid pharmacokinetic parameters after single- dose administration of intravenous, oral, or rectal acetaminophen. Pain Pract. 2012; 12: 523-532.
- Pettersson PH, Jakobsson J, Owall A. Intravenous acetaminophen reduced the use of opioids compared with oral administration after coronary artery bypass grafting. J CardiothoracVascAnesth. 2005; 19: 306-309.
- Ohnesorge H, Bein B, Hanss R, Francksen H, Mayer L, Scholz J, et al. Paracetamol versus metamizol in the treatment of postoperative pain after breast surgery: a randomized, controlled trial. Eur J Anaesthesiol. 2009. 26: 648-653.
- Memis D, Inal MT, Kavalci G, Sezer A, Sut N. Intravenous paracetamol reduced the use of opioids, extubation time, and opioid-related adverse effects after major surgery in intensive care unit. J Crit Care. 2010; 25: 458-462.
- Atef A, Fawaz AA. Intravenous paracetamol is highly effective in pain treatment after tonsillectomy in adults. Eur Arch Otorhinolaryngol. 2008; 265: 351-355.
- Cakan T, Inan N, Culhaoglu S, Bakkal K, Basar H. Intravenous paracetamol improves the quality of postoperative analgesia but does not decrease narcotic requirements. J NeurosurgAnesthesiol. 2008; 20: 169-173.
- Alhashemi JA, Daghistani MF. Effect of intraoperative intravenous acetaminophen vs. intramuscular meperidine on pain and discharge time after paediatric dental restoration. Eur J Anaesthesiol. 2007; 24: 128-133.