Case Report
Austin J Anesthesia and Analgesia. 2014;2(3): 1018.
Giant Left Ventricular Pseudoaneurysm
Marek Brzezinski*1, John D Mitchell2, Donald D. Glower3, Jasleen Kukreja4, Paul S. Pagel5, Katherine Grichnik6
1Department of Anesthesia and Perioperative Care,University of California, USA
2Department of Anesthesia and Critical Care, Harvard University, USA
3Department of Surgery, Duke University, USA
4Department of Surgery, University of California, USA
5Medical College of Wisconsin, Anesthesia Service Clement J. Zablocki Veterans Affairs Medical Center Milwaukee West Indies
6Department of Anesthesiology, Duke University, USA
*Corresponding author: Marek Brzezinski, MD PhD, Department of Anesthesia and Perioperative Care, University of California, San Francisco, VA Medical Center, 4150 Clement Street, San Francisco, CA 94121.
Received: March 26, 2014; Accepted: April 10, 2014; Published: April 15, 2014
Abstract
A 70-year-old woman underwent left ventricle (LV) pseudoaneurysm resection and LV wall repair with a Hemashield patch (4 x 6 cm). The LV pseudoaneurysm represented an incidental finding in patient status post myocardial infarction two years prior. The patient underwent surgical pseudoaneurysm resection with a patch, and mitral valve annuloplasty. The wall of the pseudoaneurysm consisted of fibrous tissue and partially organized thrombus. Her postoperative course was uncomplicated. Transesophageal echocardiogram (TEE) is an important imaging technique in the management of pseudoaneurysm repair.
Keywords: Imaging; Ultrasound; Heart Pathology; Aneurysm.
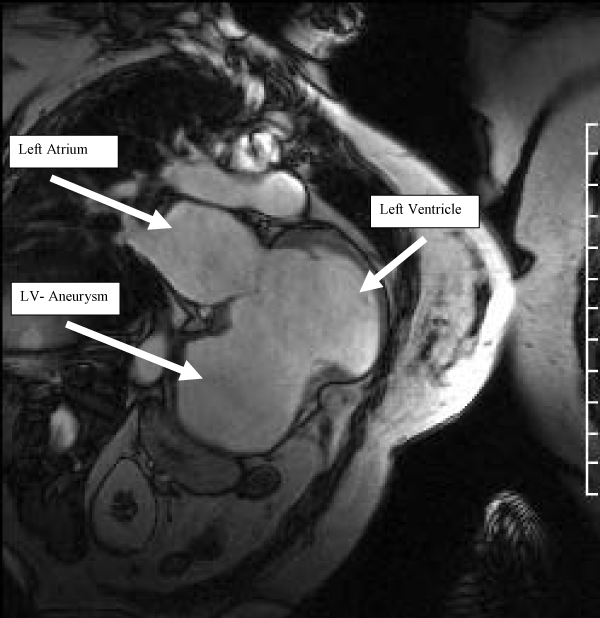
A 70 year-old woman was admitted for surgical repair of a giant left ventricular pseudoaneurysm that occupied the majority of the LV inferior wall (Figures 1 and 2). The patient initially presented two years before the current admission with an inferior wall myocardial infarction resulting from acute occlusion of the right coronary artery. A percutaneous coronary angioplasty of the occluded vessel was successful, but the inferior wall ruptured shortly after the procedure and an emergent patch repair was required to close the defect. The patient recovered from this incident, but subsequently developed a large inferior wall pseudoaneurysm that was incidentally detected on a magnetic resonance imaging (MRI) scan (Figure 1) that had been performed for an unrelated problem. The MRI demonstrated that the neck of the pseudoaneurysm was 5.9 cm in diameter whereas the body measured 8.8 x 9.9 cm in maximum dimension. A chest radiograph revealed a markedly enlarged cardiac silhouette (Figure 2). The intraoperative transgastric transesophageal echocardiography (TEE) short-and long-axis images showed a giant LV pseudoaneurysm that encompassed the entire basal and mid-myocardial segments of the inferior wall (Figures 3A and 3B). Left ventricular ejection fraction was reduced concomitant with moderate tricuspid (not shown) and severe mitral valve regurgitation (Figure 4). The patient was taken to the operating room for repair of the LV pseudoaneurysm. During cardiopulmonary bypass, the pseudoaneurysm was resected, the remaining large LV defect was closed using a 4 x 6 cm Hemashield® (Maquet Cardiovascular, Wayne, NJ) patch, and a mitral valveannuloplasty was performed. Gross inspection of the resected pseudoaneurysm revealed fibrous tissue and partially organized thrombus. The patient separated from cardiopulmonary bypass using inotropic support. A repeat TEE examination demonstrated the patch repair (Figures 5A and 5B) and minimal residual mitral valve regurgitation (not shown). The patient's postoperative course was unremarkable.
Figure 1: Magnetic resonance imaging study showing the giant left ventricular pseudoaneurysm of the inferior wall.
Figure 2: Posterior-anterior chest radiograph showing markedly enlarged cardiac silhouette resulting from the giant left ventricular pseudoaneurysm. Despite the significant pathology, the patient was able to complete activities of daily living without any chest pain or shortness of breath, with only infrequent episodes of mild exertional fatigue. She denied any palpitations or orthopnea.
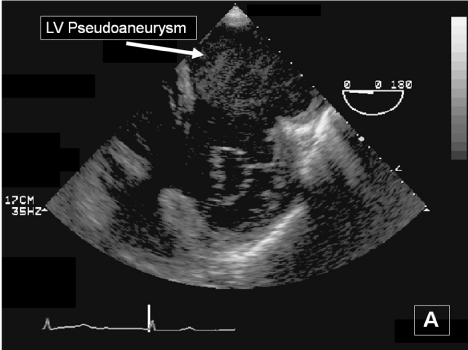
Figure 3a: Transgastric basal short- and long-axis transesophageal echocardiography images obtained immediately below the mitral valve annulus showing the giant inferior wall left ventricular pseudoaneurysm.
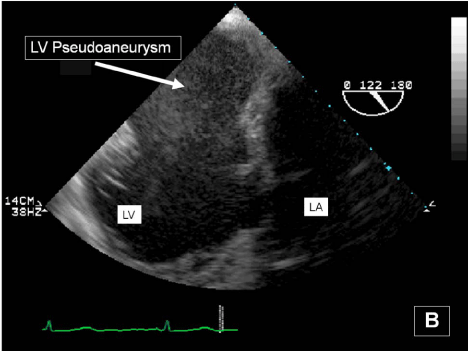
Figure 3b: Transgastric basal short- and long-axis transesophageal echocardiography images obtained immediately below the mitral valve annulus showing the giant inferior wall left ventricular pseudoaneurysm.
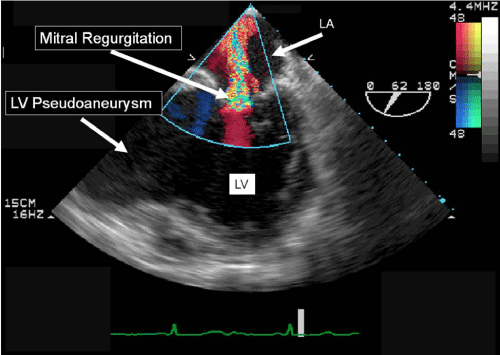
Figure 4: Midesophageal bicommissural transesophageal echocardiography image showing severe mitral regurgitation and the giant inferior wall left ventricular pseudoaneurysm.
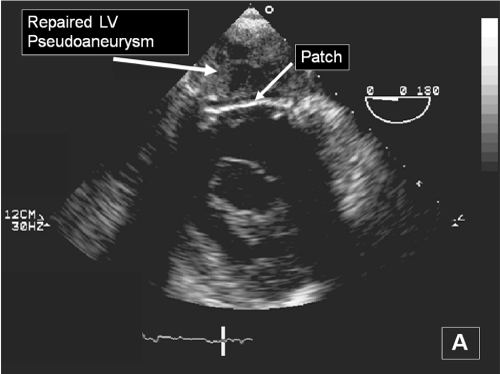
Figure 5a: Transgastric basal short- and long-axis transesophageal echocardiography images showing patch repair of the giant inferior wall left ventricular pseudoaneurysm.
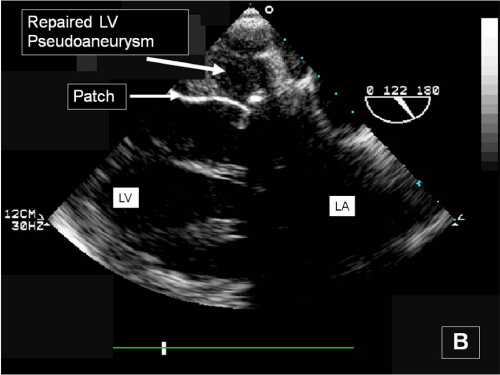
Figure 5b: Transgastric basal short- and long-axis transesophageal echocardiography images showing patch repair of the giant inferior wall left ventricular pseudoaneurysm.